
By Xam Riche on March 26, 2026 • 14 min read
This article is for informational and educational purposes only and does not constitute medical advice. Always consult with a registered dietitian, gastroenterologist, or other qualified medical professional before making significant dietary changes or starting treatment.

Bloating is not always just a food-trigger story. Sometimes the bigger driver is slower stool movement, harder stools, straining, or the feeling that you never fully emptied in the first place. When that is the pattern, treating the backup often helps more than tightening the diet again.
Short answer: constipation can make bloating feel louder by increasing pressure, fullness, incomplete evacuation, and the sense that meals are sitting badly when the bigger problem is stool backup.
This page is for you if your bloating seems to track with hard stools, straining, incomplete evacuation, or pressure that eases after a better bowel movement.
Use a different page first if your main clue is a broader food-trigger pattern, a classic IBS-style low-FODMAP question, or a supplement comparison. Those fit how to reduce bloating, IBS-C and low FODMAP, or synbiotics for constipation better.
If your stomach feels full, tight, noisy, or visibly distended, it is easy to blame the last meal.
Sometimes that is true.
But sometimes the more useful question is not "What did I eat?" It is "What is my bowel pattern doing right now?"
That distinction matters. The broader bloating guide covers many possible causes, but this article focuses on one of the most commonly underweighted ones: the link between constipation and bloating.
The goal here is practical. We will sort the pattern, cover what to change first, and show when the situation starts looking less like occasional constipation and more like IBS-C or a broader digestive workup.
This page is explaining a stool-backup and pressure pattern:
This page is not mainly explaining:
If one of those sounds closer, route to IBS-C and low FODMAP, low FODMAP for beginners, or functional dyspepsia.
It can.
NIDDK defines constipation more broadly than "not going often enough." Symptoms can include fewer than three bowel movements per week, hard or lumpy stools, painful or difficult passage, and the feeling that not all stool has passed 1.
That last part matters because many people still have bowel movements and still feel constipated.
If you often notice:
then constipation may be part of the bloating story even if you are not going several days without stool.
NICE uses similar language in IBS guidance. It notes that altered stool passage can include straining and incomplete evacuation, and that bloating, distension, tension, or hardness often sit in the same symptom cluster 2.
That does not mean every bloated reader has IBS.
It means this: if stool is hard to move, incomplete, or inconsistent, the bowel pattern deserves attention before you assume every flare is coming from one "wrong" food.
If you are blaming fruit, yogurt, salads, or whole grains first, read why healthy foods still cause bloating to separate food-trigger patterns from stool-backup patterns.
This is the part many readers intuit, but do not always hear explained clearly.
Rome Foundation notes that bloating frequently accompanies constipation and that treating constipation often improves bloating 3. That is the core connection this article is built around.
In plain language, when stool is moving more slowly or sitting longer in the system, pressure and fullness can feel louder. Gas can feel harder to clear. Meals that would normally feel manageable can suddenly feel heavier, tighter, or more distending.
That pattern is also supported in the research literature. A PubMed-indexed study found that functional constipation and constipation severity were both associated with more severe bloating 4.
The practical mistake is easy to make:
you feel bloated, assume the problem is only the food, cut more foods, and never really address the stool pattern underneath the pressure.
That is one reason readers can end up stuck between two half-solutions:
If food combinations still matter on top of that, the next useful layer is FODMAP stacking. But stool backup should be ruled in or out first, because it can make every meal feel noisier than it really is.
This is not about self-diagnosing everything from home. It is about noticing patterns that make your next step smarter.
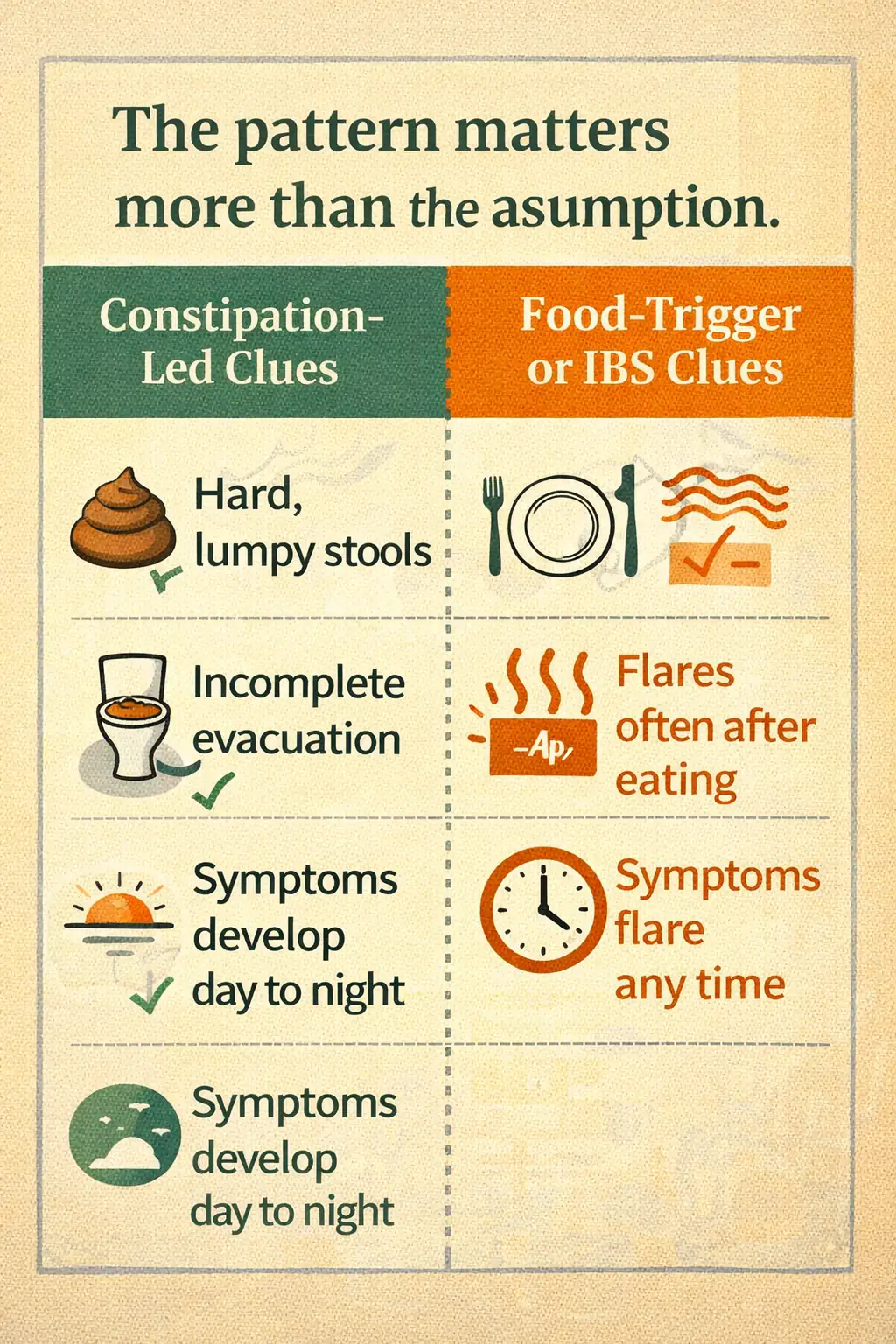
If the overlap feels genuinely hard to separate, the bigger map is IBS, SIBO, and food intolerance. If the pattern is clearly chronic constipation plus bloating and abdominal pain, then an IBS-C and low-FODMAP strategy may become more relevant.
The main point is not to make you over-analyze every day. It is to stop using food restriction as the default answer before the constipation pattern has even been addressed.
| Pattern | More likely means | Best next move |
|---|---|---|
| Hard stools, straining, incomplete evacuation | constipation-led pressure | support stool movement first |
| Pressure improves after a better bowel movement | stool backup is a major factor | stay with constipation-first strategy |
| Symptoms clearly spike after certain foods even when bowels are okay | food-trigger or IBS overlap | widen into food and IBS review |
| Vomiting, severe pain, inability to pass gas, blood | escalation territory | stop self-troubleshooting |
[!TIP] Track It Clearly: Bloating Pattern Tracker Use it for several days if you are stuck between "this must be food" and "this feels more like stool backup."
The first move is usually not "cut more foods."
The first move is usually to make stool movement easier and the daily pattern less chaotic.
NICE recommends regular meals, avoiding long gaps between eating, and getting adequate fluid intake in IBS care 5. That matters here too. Random grazing, skipped meals, and long gaps can make the whole pattern harder to read.
Try replacing:
NIDDK says to eat enough fiber, drink enough liquid to help the fiber work better, and add fiber gradually rather than all at once 6.
That gradual part matters. A sudden jump can make bloating louder before things settle.
For readers with IBS-type symptoms, the type of fiber matters too. NICE discourages insoluble fiber like bran for IBS and instead favors soluble-fiber options such as ispaghula or foods like oats 7. NIDDK's IBS nutrition guidance similarly says soluble fiber appears more helpful and that too much fiber too fast can trigger gas and bloating 8.

NIDDK recommends regular physical activity and bowel training, including trying to have a bowel movement at the same time each day, often 15 to 45 minutes after breakfast 9.
That is not glamorous advice, but it is high-value advice.
Small changes matter:
The 2023 joint AGA / ACG guideline recommends fiber supplementation and PEG for adults with chronic idiopathic constipation 10. NIDDK also lists osmotic agents such as Miralax among common treatment options 11.
That does not mean this article is telling you to self-prescribe a whole treatment stack.
It means you are allowed to stop pretending diet is the only respectable tool. If the basics are not enough, clinician-guided treatment belongs in the conversation. And if the next question is whether a microbiome supplement belongs in that conversation too, use our guide to synbiotics for constipation to compare prebiotics, probiotics, and combo products without defaulting to marketing logic.
| If This Is Happening | Change This First | Why |
|---|---|---|
| You are grazing but still feel backed up | move to regular meals and more fluid | better rhythm helps stool movement |
| You cut many foods and feel more beige than better | add gradual fiber and more produce | prevents accidental low-fiber over-restriction |
| You only focus on food lists | add movement and bowel timing | constipation is not only a food issue |
| You already tried the basics without progress | discuss PEG or clinician-guided next steps | diet is not the only tool |
[!IMPORTANT] Start Here First: Constipation-Bloating First-Step Checklist Use it before you tighten your diet or assume the last meal explains everything.
If you already did tighten the diet and still feel stuck, the next read is Low FODMAP not working, especially if hidden ingredients or a bigger diagnostic mismatch may also be involved.
This is where many people accidentally make the pattern worse.
They move toward "safe" beige foods:
Those foods are not automatically wrong. But if they crowd out produce, fluid, meal volume, and a more intentional fiber pattern, the day can become more constipating by default.
What usually helps more:
NHS specifically lists water, smaller meals, exercise, and soluble-fiber foods such as oats or linseed among its practical tips for bloating when constipation is involved 12.
That does not mean the article should become a giant constipation food list. The better frame is meal structure.
Examples:
If you are already inside a low-FODMAP phase and need food-specific support, use the low-FODMAP foods guide and, if needed, the 7-day meal plan. But the goal here is still broader than low FODMAP alone: get the stool pattern working with you, not against you.
Not every reader with constipation and bloating needs low FODMAP.
But some do.
If the pattern is chronic, recurring, and tied to abdominal pain, altered bowel habit, incomplete evacuation, and repeat symptom flares, the situation may be closer to IBS-C than occasional constipation.
That is where the next layer changes.
NICE says low FODMAP belongs after general lifestyle and dietary advice if IBS symptoms persist, and that it should be given by a professional with dietary expertise 13. NIDDK similarly presents low FODMAP as one IBS diet strategy among several, alongside fiber changes 14.
That is why this article keeps low FODMAP later, not first.
If the pattern really does look IBS-C-like, move next into:
The key is sequence:
This is where precision matters.
NIDDK advises prompt medical care for constipation with rectal bleeding, blood in stool, constant abdominal pain, inability to pass gas, vomiting, fever, lower back pain, or weight loss without trying 15. NHS likewise flags bloating with vomiting, fever, severe stomach pain, or inability to pee, poo, or fart as situations that should not stay in self-management mode 16.
A practical split looks like this:
| Situation | Best next move |
|---|---|
| Mild recurring bloating with a clear constipation pattern | self-care and tracking |
| Chronic constipation and bloating that keeps returning | routine clinician review |
| Vomiting, blood, fever, severe pain, inability to pass gas | urgent medical review |
If the pattern has shifted from routine backup into cramping waves, progressive distention, or more constant pain, review our guide to bowel obstruction pain patterns.
If the pattern is messy and you are not sure whether it is IBS, SIBO, or another digestive issue, go wider with SIBO vs IBS vs food intolerance rather than guessing from symptoms alone.
If you want the shortest version, here it is:
That sequence matters because it prevents two common mistakes at once:
If your next step needs to stay broad, use the bloating guide. If the pattern looks more like IBS-C, move into IBS-C and low FODMAP. If you already restricted food and still feel stuck, go straight to Low FODMAP not working. For a practical morning routine, use the constipation-first breakfast strategy to test fiber, fluids, coffee, and timing without changing the whole diet at once.
Xam Riche is a gut health solopreneur and founder of YourFitNature, dedicated to helping people navigate digestive wellness through evidence-based information and personal experience. After years of struggling with IBS and bloating, Xam discovered the transformative power of the low FODMAP diet and now shares practical, science-backed guidance to help others find relief. While not a medical professional, Xam combines extensive research with lived experience to create accessible, empowering resources for the gut health community. Learn more about our mission
As an affiliate, we may earn from qualifying purchases.
Showing 10 of 92