
By Xam Riche on April 13, 2026 • 14 min read
This article is for informational and educational purposes only and does not constitute medical advice. Always consult with a registered dietitian, gastroenterologist, or other qualified medical professional before changing your treatment plan or starting a new therapy.

If a few bites make you feel uncomfortably full, nauseated, or painfully aware of your upper stomach, generic IBS advice can feel incomplete. Functional dyspepsia is a real gut-brain disorder with its own symptom patterns, overlap zones, and treatment logic. The good news: once the pattern is clearer, the next steps usually get clearer too.
This page answers a specific bridge question: when does an upper-GI pattern fit functional dyspepsia better than another round of generic IBS advice?
The short answer is that functional dyspepsia becomes more plausible when the main story is early fullness, post-meal heaviness, nausea, or upper-abdominal pain and burning, especially when lower-GI IBS framing never fully explains the picture.
This guide is for readers whose symptoms feel meal-related and upper-abdominal. If your main issue is still lower-GI bloating or bowel-pattern confusion, start with how to reduce bloating or SIBO vs IBS vs food intolerance.
You eat what looks like a normal meal. Maybe even a small one. Then halfway through, your stomach acts like you already overdid it.
You feel full too fast. Heavy. Queasy. Sometimes there is burning high in the abdomen. Sometimes there is pressure that makes you wonder whether this is reflux, IBS, anxiety, or just a bad run of digestion.
That confusion is common. And it is one reason so many people spend months or years trying lower-GI solutions that do not fully explain what is happening. If you already went down the food-first path and still feel stuck, start with our guide to what to do when low FODMAP is not working.
Here is the truth: functional dyspepsia is not just random indigestion. Most chronic indigestion ends up being diagnosed as functional dyspepsia, which current NIDDK guidance classifies as a disorder of gut-brain interaction 1.
That matters because the label changes the conversation. Instead of asking only what food upset your stomach, you can ask a better question:
Which symptom pattern am I actually dealing with, and which treatment lever fits it best?
This guide will help you sort the pattern and the next-step options more cleanly.
Functional dyspepsia, often shortened to FD, describes chronic upper-GI symptoms that do not have a clear structural explanation on routine testing. The symptom cluster usually includes upper-abdominal pain or burning, early satiety, post-meal fullness, nausea, bloating, and belching 2.
The important part is not just the label. It is the location and pattern.
FD is usually an upper-gut story. The discomfort tends to sit higher in the abdomen and often flares during or soon after eating. That makes it different from the classic IBS pattern, where lower-abdominal pain and bowel habits tend to dominate.
Heartburn can exist alongside FD, and so can reflux. But they are not automatically the same condition. That is one reason upper-abdominal symptoms can feel so messy in real life.
Bottom line: if your main complaint is that meals feel too heavy, too early, or too painful in the upper stomach, the FD framework may fit better than another round of generic bloating advice.
If you want the bigger signaling map behind hunger, satiety, and why meal experience can feel biologically mixed before you narrow into FD, use gut-brain signaling and appetite.
If you want the microbiome-facing mechanism shelf behind the same gut-brain language before you come back to an upper-GI pattern, use microbiome signaling explainer.
The simplest distinction is this:
That sounds tidy. Real life is not.
A meta-analysis found that FD and IBS overlap is common enough that roughly one in three patients across the relevant functional GI groups may fit both patterns rather than only one 3. So if you have early fullness and post-meal discomfort plus urgency, constipation, or lower-abdominal pain, that does not mean you failed to describe your symptoms correctly. It may mean the pattern is mixed.
That is why symptom mapping matters more than label loyalty.
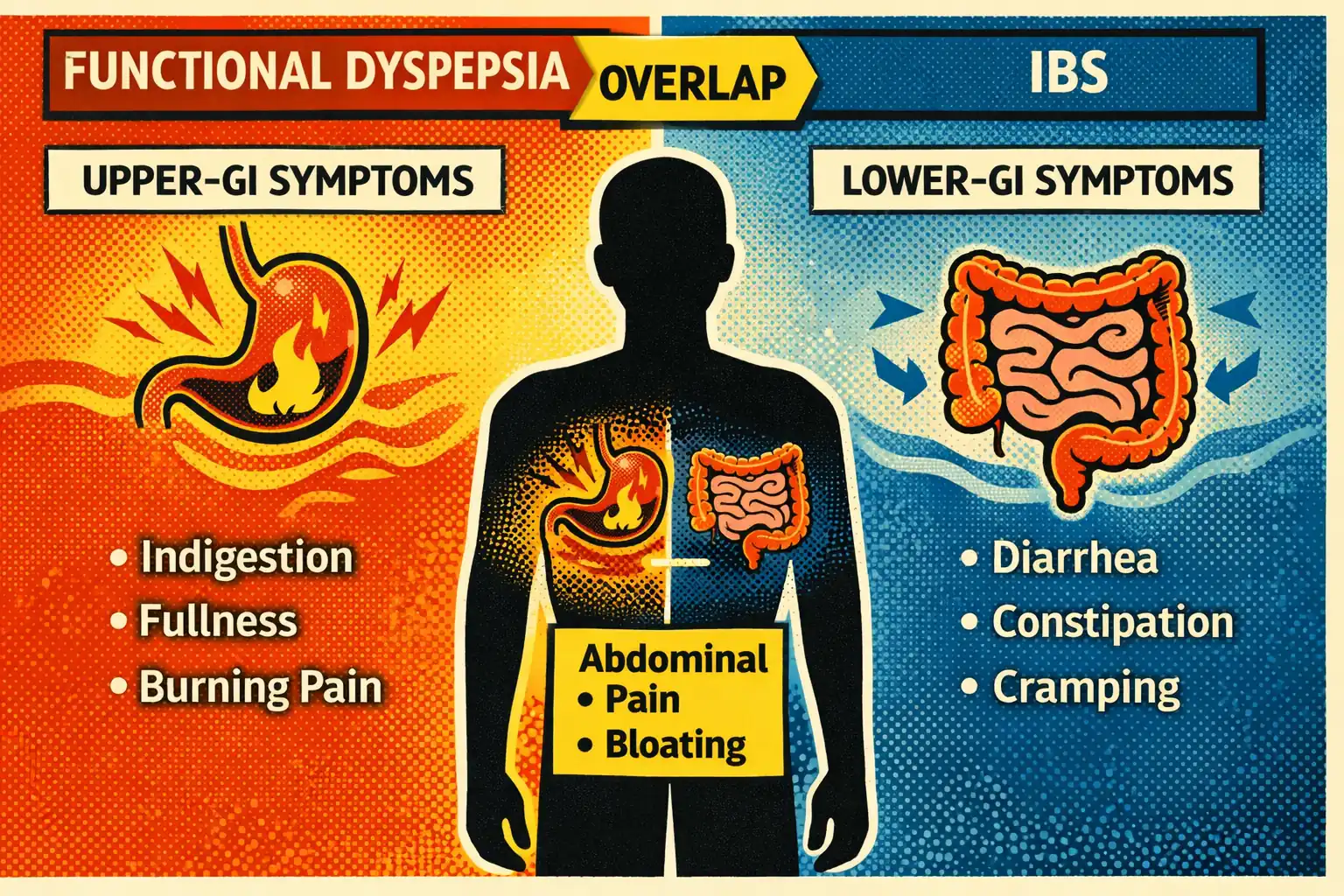
If you are still sorting whether this sounds more like IBS, SIBO, or another food-driven pattern, use our side-by-side guide to IBS vs other gut patterns.
Here is a fast comparison:
| Pattern | Functional Dyspepsia | IBS |
|---|---|---|
| Main symptom location | Upper abdomen | Lower abdomen / bowel pattern |
| Typical meal issue | Early fullness, heaviness, nausea | Urgency, diarrhea, constipation, lower bloating |
| Pain pattern | Epigastric pain or burning | Lower abdominal pain often tied to bowel habit |
| Best fit question | Why do small meals feel like too much? | Why are bowel habits and lower-GI symptoms so unstable? |
Use that table as a direction finder, not a diagnostic verdict.
FD gets easier to understand once you know the two main subtype labels:
Those are not just academic categories. They help explain why two people can both have FD and still sound very different.
If your pattern is mostly PDS, you may say things like:
If your pattern is more EPS, you may say:
The Rome IV epidemiology work continues to support the value of these subgroups, even though some people fit a mixed pattern 4.
That mixed pattern is important. It means you do not need to force yourself into a neat box before the treatment conversation starts.
There is no single explanation that fits every FD case.
Current higher-level sources point to a mix of mechanisms that may matter in different people:
H. pylori or other conditions may still need evaluation firstNIDDK explicitly lists problems with stomach accommodation, pain from normal stomach function, duodenal inflammation or sensitivity, and anxiety or depression among factors that may play a role 5.
That does not mean the symptoms are imagined.
It means the gut-brain system can make ordinary digestive signals feel louder, more uncomfortable, or harder to recover from. If that idea still feels vague, read our broader explainer on the gut-brain axis.
There is also active research on gut-brain and microbiota mechanisms in FD, including duodenal dysbiosis, but that work is still better treated as mechanistic context than as a simple consumer checklist 6.
This is where many articles get lazy. They dump every treatment into one list and leave you guessing.
The better way to think about FD treatment is pattern first, tool second.
If H. pylori is present, treatment matters. If the pattern suggests another
condition entirely, that matters too. NIDDK includes H. pylori treatment as a
standard part of dyspepsia management when relevant, and its diagnosis guidance
also makes clear that clinicians may use further testing when another cause
needs to be ruled out
7
8.
PPIs or H2 blockers tend to make the most intuitive sense when upper-abdominal burning or acid-sensitive symptoms are central. They are not the universal answer, but they are a logical part of the conversation 9 10.
When the loudest story is early satiety, meal heaviness, or nausea after small amounts of food, prokinetic-style conversations and meal-structure changes often make more sense than defaulting straight to pain-focused treatment 11.
If you are considering a food-first comfort step while you sort the pattern, use this anti-hype comparison of ginger tea vs ginger supplements as a narrow fit check for nausea or mild meal discomfort, not as a replacement for the FD treatment conversation.
This is where the language needs to stay precise.
Neuromodulators do not mean "your symptoms are psychological." In FD, they are used because pain signaling and symptom amplification can be part of the problem.
The 2022 BSG guideline and a 2020 network meta-analysis both support TCAs as one of the more credible drug categories in FD, while SSRIs look less convincing 12 13.
A multicenter randomized trial also found that amitriptyline outperformed escitalopram and placebo for adequate relief, with the clearest benefit in pain-predominant FD 14.
That is useful because it tells you not to flatten all antidepressant-class medications into the same story.
If the same pain-volume problem seems lower-GI or IBS-dominant rather than upper-stomach dominant, use visceral hypersensitivity in IBS to separate amplified gut sensation from dyspepsia pattern-matching.
Psychological therapies have supportive, though still not perfect, evidence in FD. Recent reviews suggest they can improve symptoms and anxiety, especially when the gut-brain loop is clearly part of the pattern 15 16.
If stress-sensitive symptom amplification is obvious, read what the evidence actually says about gut-directed hypnotherapy.
[!TIP] Download: Functional Dyspepsia Doctor Discussion Guide Use this before your next appointment to sort which treatment conversation actually fits your pattern.
Many readers land here expecting a diet fix. That makes sense. But this is where restraint matters.
A 2025 critical review concluded that structured diet changes, including some low-FODMAP-style strategies, may help a subset of FD patients, especially when PDS, bloating, or IBS overlap is present. But the evidence is still mixed and heterogeneous 17.
That means the practical diet advice should stay simple first:
If upper-GI discomfort seems tied to coffee, tea, or stimulant drinks, use coffee, tea, and gut symptoms before treating every warm drink as a gut-health choice.
If nausea, early fullness, or heavy upper-GI discomfort is the practical symptom you want to test gently, use ginger for nausea, fullness, and digestive discomfort as a symptom-tool route instead of turning the whole pattern into another broad food restriction plan.
If bloating and lower-GI overlap are strong enough that you are tempted to make food the whole story again, pause and review our guide to what to do when food changes are not enough.
[!TIP] Download: Functional Dyspepsia Symptom Pattern Checklist Print this if you keep switching between 'maybe IBS,' 'maybe reflux,' and 'maybe I just ate wrong.' It helps you sort the pattern before you over-restrict again.
FD is a useful framework. It is not permission to ignore warning signs.
Seek more evaluation if you have:
If the warning-sign question is mainly lower-GI bleeding, anemia, or a bowel pattern that no longer feels like routine IBS, use IBS vs colorectal warning signs as the more relevant comparator.
Those are not "maybe later" symptoms. NIDDK specifically flags chest pain, trouble swallowing, frequent vomiting, black stools, severe constant abdominal pain, and unintentional weight loss as reasons to get medical help rather than assuming the pattern is uncomplicated FD 18 19.
It is also worth stepping back if the story may fit something else better, such as peptic ulcer disease, GERD, gastroparesis, medication side effects, or a mixed lower-GI pattern that still needs IBS workup.
That does not mean you should panic. It means you should avoid squeezing every symptom into the FD label when the pattern no longer fits.
Functional dyspepsia becomes much less confusing once you stop asking one big vague question and start asking a few smaller useful ones:
Bottom line:
Start here if you need a next move:
If early fullness is making appetite low and you need a smaller first-meal route, use IBS safe foods when appetite is low alongside this upper-GI symptom map.
Xam Riche is a gut health solopreneur and founder of YourFitNature, dedicated to helping people navigate digestive wellness through evidence-based information and personal experience. After years of struggling with IBS and bloating, Xam discovered the transformative power of the low FODMAP diet and now shares practical, science-backed guidance to help others find relief. While not a medical professional, Xam combines extensive research with lived experience to create accessible, empowering resources for the gut health community. Learn more about our mission
As an affiliate, we may earn from qualifying purchases.
Showing 10 of 143