
By Xam Riche on April 29, 2026 • 10 min read
This article is for informational and educational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional before using microbiome or gut-brain information to make diagnosis or treatment decisions.
The phrase microbiota-gut-brain axis shows up everywhere now. One headline says gut microbes shape mood. Another says they influence cravings. A third says dysbiosis explains IBS. The term starts sounding important and fuzzy at the same time. The useful move is not to reject the phrase. It is to unpack it into the signaling lanes it actually describes.
Short answer: the microbiota-gut-brain axis is the signaling network through which gut microbes, gut tissues, and the nervous system influence one another through neural, immune, endocrine, and metabolite pathways 1 2. It is real, useful, and easy to overclaim.
Use a different page first if your main need is practical stress relief, an appetite-signaling bridge, or a narrow IBS-D mechanism. Start with the practical gut-brain axis, the gut-brain signaling and appetite bridge, or serotonin and IBS-D.
Health note: this page explains mechanisms and route choices. It is not a diagnosis and it is not a substitute for clinician-guided evaluation.
The phrase sounds as if it should describe one direct cable from microbes to the brain. That is not the best way to understand it.
The microbiota-gut-brain axis is a translated signaling system. Microbes change the gut environment. Gut tissues detect and respond to those changes. Signals then move through host pathways that can affect motility, sensation, appetite, stress reactivity, and the way gut signals are interpreted 3.
That translation step matters. It protects you from the most common online mistake: acting as if gut bacteria directly control mood, appetite, pain, and behavior in one simple way.
It also explains why the same term shows up in several different kinds of articles. Some writers use the axis to talk about stress-sensitive digestion. Some use it to talk about appetite and food reward. Others use it for motility, pain amplification, or metabolite signaling. Those uses are not automatically wrong. They are only wrong when one lane is presented as if it were the whole map.
That is the most practical reason to read a page like this one. If you can see the map, you can stop expecting one probiotic, one stool test, or one social media trend to explain every gut-brain pattern you experience.
The easiest way to understand the axis is to split it into lanes.

The neural lane includes the enteric nervous system, sensory cells in the gut, and vagal pathways. This does not mean bacteria directly phone the brain. It means microbial activity can alter conditions that are sensed and translated by host tissues and nerves 4.
NIDDK's research update on direct gut-brain communication is useful because it shows that specialized gut sensory cells can pass information to the nervous system quickly 5.
That is editorially useful because it stops the field from sounding magical. The gut can influence the brain quickly in some contexts, but that speed still depends on real host tissues doing the translation work. The microbiome may modulate the environment around those systems. It is not the same as saying the microbiome is the only actor in the scene.
Microbes matter because they change the gut environment the immune system and epithelial barrier have to manage. When that environment shifts, local immune tone, barrier behavior, and sensory signaling can shift with it 6 7.
This helps explain why the field shows up in conversations about stress, symptom sensitivity, and gut discomfort without proving that one product or one protocol is the fix.
This lane also helps explain why the term "dysbiosis" gets used so loosely. Readers hear about barrier changes, inflammation, or immune signaling and assume that any uncomfortable gut pattern proves that their microbiome is damaged in one simple way. The better conclusion is narrower: host-microbe interactions can shape how loud or stable the gut environment feels, but that still has to be interpreted in context.
Tryptophan metabolism has become one of the cleaner bridges linking the gut microbiome to gut-brain homeostasis 8. A 2015 paper also showed that indigenous gut bacteria regulate host serotonin biosynthesis 9.
That does not mean the microbiome explains every serotonin story. It does mean the microbiome belongs in the same signaling conversation as motility, secretion, and gut sensation.
This is especially important in gut-health writing because serotonin language easily gets flattened into mood language. In the gut, serotonin is also part of motility and sensation. So when the microbiome is brought into a serotonin discussion, the useful interpretation is usually about gut signaling, not about claiming that one microbiome intervention will rewrite a whole mental-health picture.
If you want the narrower cell-level bridge between microbial or luminal cues, enterochromaffin-cell serotonin release, and downstream urgency or pain routes, read enterochromaffin cells, serotonin, and gut pain signaling.
Short-chain fatty acids are one of the clearest examples of a microbial lane turning into host-facing physiology. A 2022 review treats SCFAs as important gut-brain signaling molecules with both direct and indirect effects 10.
But SCFAs are still only one lane. If you mainly want the metabolite shelf, use short-chain fatty acids. If you want the upstream ecological input layer, use fiber diversity and microbiome resilience or polyphenols and the gut microbiome.
That ranking matters because the metabolite lane is one of the easiest places for translation to drift. It is fair to say metabolites help explain how gut microbes can affect host physiology. It is not fair to say that hearing one metabolite name automatically tells you which food, supplement, or protocol is right for you next.
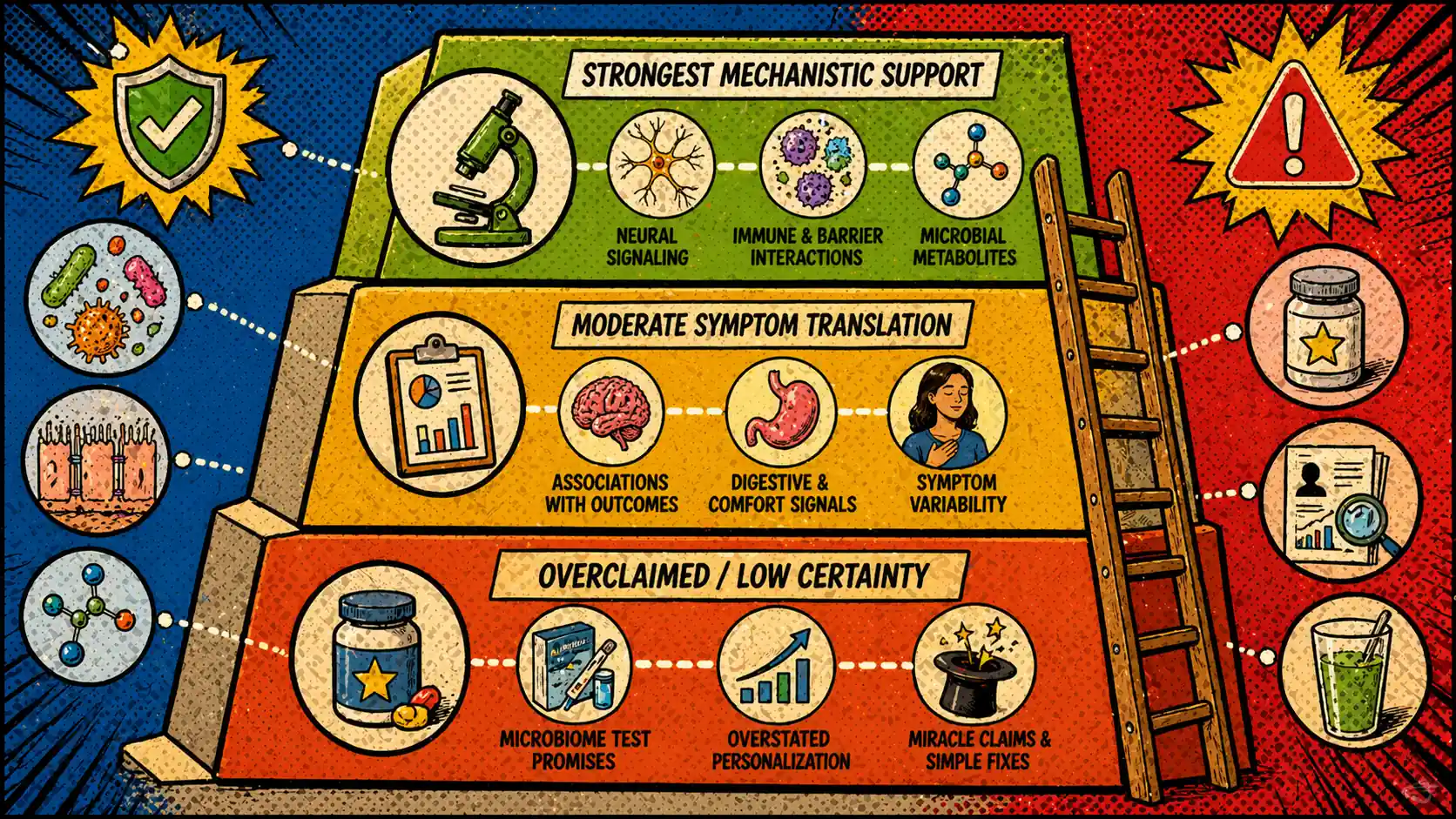
| Evidence level | What the field can say more confidently | What it should not quietly imply |
|---|---|---|
| Strongest | The microbiota-gut-brain axis is a real signaling framework with neural, immune, endocrine, and metabolite lanes | One lane explains the whole person |
| Moderate | Microbiome-linked signaling may shape appetite, motility, stress reactivity, and symptom sensitivity | Every symptom pattern maps neatly to one intervention |
| Weakest | A claim may sound biologically plausible | One stool test or one probiotic gives a reliable universal answer |
The middle row is where most confusion lives. Readers often hear a biologically plausible story and assume the practical action should now be obvious. But a mechanism can be meaningful without being decision-complete. That is why a lot of microbiome content feels persuasive and still does not reliably tell you what to change tomorrow morning.
This is also why review-heavy mechanism pages can still be useful when they are honest. Their job is to help you interpret claims, not to impersonate a clinician or a treatment algorithm.
Download: Microbiome-Gut-Brain Signal Ladder Use this one-page ladder when a microbiome claim sounds convincing but you need to sort mechanism from action.
The practical next page is usually stress-bloating through the gut-brain axis, not more abstract mechanism reading.
Use gut-brain signaling and appetite. It takes the body-state experience much further than this broader mechanism page.
Use serotonin and IBS-D. That page takes one signaling lane from this broader map and applies it to a more precise clinical pattern.
Use visceral pain amplification when threat sensitivity and chronic gut pain are louder than general microbiome-curiosity.
If you need the plain-language version of why ordinary gut signals can feel painful, start with visceral hypersensitivity in IBS before moving into deeper mechanism pages.
That route logic is what keeps the axis from becoming a vague all-purpose idea. The field is broad, but readers still need narrower next steps. A good mechanism page should reduce confusion, not extend it.
When you see a microbiome claim, ask:
Two extra cautions are worth keeping in mind.
First, association is not the same as direction. If one microbial pattern shows up in a group with a certain symptom, that does not automatically prove the microbe pattern caused the symptom or that changing it will reverse the whole experience.
Second, a useful map is not the same as a ready-made product decision. Readers often move too quickly from "the axis is real" to "therefore this test, strain, or stack must be the right tool." That jump is exactly where the field gets commercialized faster than it gets clarified.
If the claim moves outside digestion into back pain or spine health, use the gut-spine claims explainer before treating a plausible mechanism like a practical treatment plan.
That anti-hype version of the field is not anti-science. It is just better at matching claims to evidence.
Download: Microbiome-Gut-Brain Next-Step Router Use this printable router when the mechanism is clear enough and the next move is choosing the right narrower page.
If symptoms come with bleeding, significant unintentional weight loss, persistent vomiting, progressive trouble swallowing, severe new abdominal pain, or a rapidly changing bowel pattern, evaluation matters more than another microbiome theory.
The same is true when the bigger problem is major fear around eating, severe distress, or a collapsing quality of life. The axis can be a useful framework, but it is not a substitute for direct support when the problem has moved beyond curiosity and into clear impairment.
The microbiota-gut-brain axis is a useful signaling framework. It helps explain why gut microbes matter through several translated lanes rather than through one direct miracle line. Use this page to understand the map, then step onto the shelf that actually matches your dominant pattern.
Xam Riche is a gut health solopreneur and founder of YourFitNature, dedicated to helping people navigate digestive wellness through evidence-based information and personal experience. After years of struggling with IBS and bloating, Xam discovered the transformative power of the low FODMAP diet and now shares practical, science-backed guidance to help others find relief. While not a medical professional, Xam combines extensive research with lived experience to create accessible, empowering resources for the gut health community. Learn more about our mission
As an affiliate, we may earn from qualifying purchases.
Showing 10 of 127