
By Xam Riche on May 1, 2026 • 10 min read
This article is for informational and educational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional or dermatologist before using microbiome or supplement content to guide diagnosis or treatment decisions.
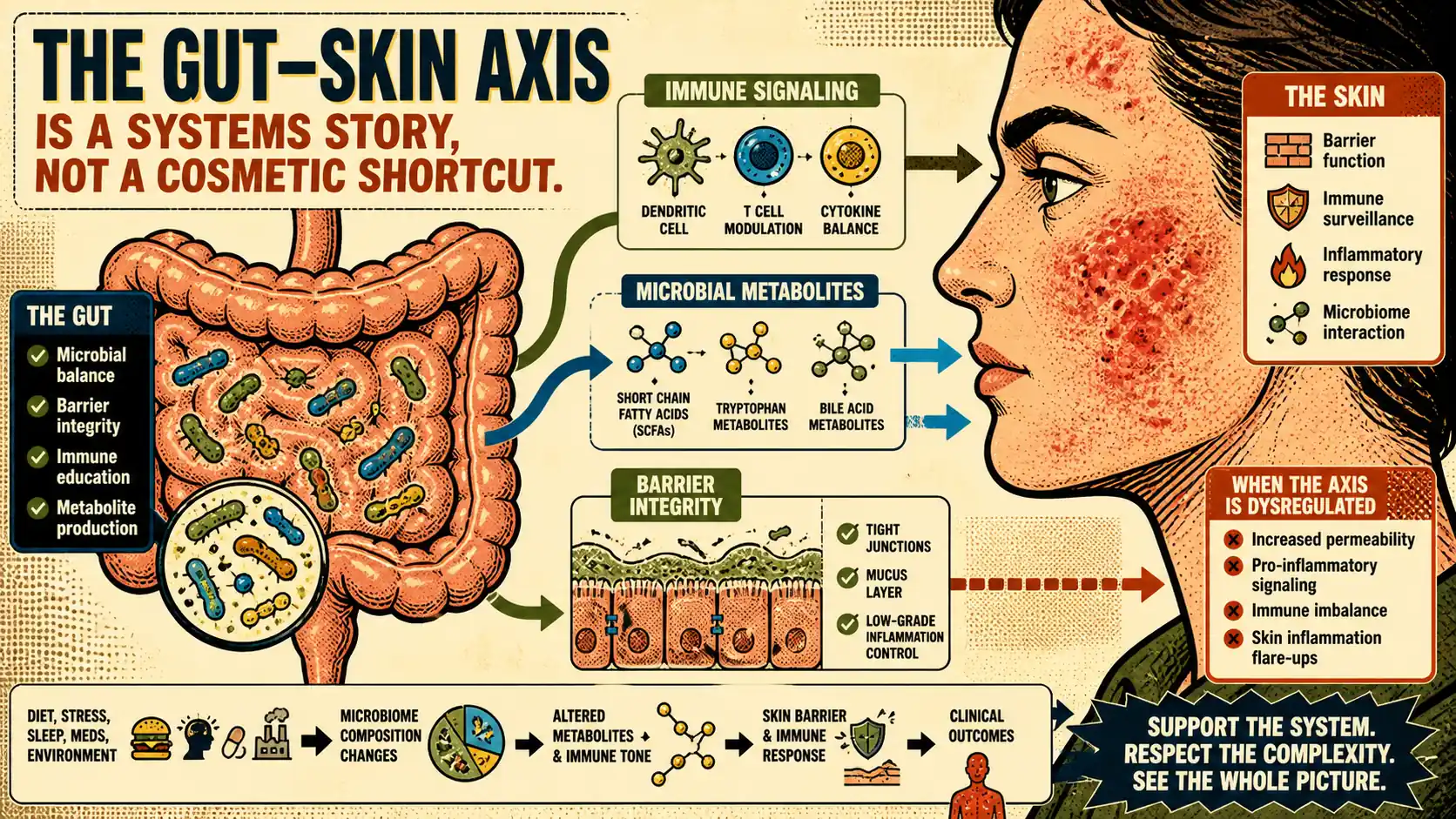
The gut-skin axis becomes confusing fast because two bad versions of the story circulate at the same time. One version turns every skin flare into a gut problem. The other treats the whole concept like wellness theater. The useful middle ground is more disciplined: gut microbes, barrier function, immune signaling, and microbial metabolites may influence inflammatory skin patterns, but that does not make probiotics a universal skin fix.
Short answer: the gut-skin axis is a real microbiome-and-immune framework, and probiotics may matter in selected inflammatory skin conditions. The practical takeaway is careful interpretation, not cosmetic hype 1 2.
This page is for you if you want to understand why eczema, acne, psoriasis, or rosacea discussions keep circling back to gut health and whether probiotic claims deserve action.
Use a different page first if your question is still about microbiome categories or product-fit basics. Start with synbiotics, probiotics, and prebiotics if you are sorting terms, or use how probiotic selection is evolving if you are trying to judge a probiotic label more intelligently.
In plain English, the gut-skin axis is the conversation between:
That framework is plausible because the gut is one of the body's main immune training environments. Reviews of the field describe bidirectional links between gut dysbiosis, immune imbalance, and skin homeostasis in inflammatory conditions 3.
The important correction is this: plausible does not mean universal.
It does not mean every acne flare is a microbiome crisis. It does not mean every eczema patient needs a probiotic. And it definitely does not mean beauty marketing suddenly became medicine.
Here is the cleanest way to picture the mechanism:
If you want the food-and-metabolite shelf underneath that diagram, use polyphenols and the gut microbiome and short-chain fatty acids and the gut microbiota before treating one organ-axis page as the entire microbiome story.
Probiotics attract attention here for the same reason they do in other microbiome conversations: they are one of the clearest attempts to modify the gut environment rather than just describe it.
The problem is that readers often collapse that into one vague promise.
The World Gastroenterology Organisation defines probiotics as live microorganisms that confer a health benefit when administered in adequate amounts, and its guidance keeps the focus on defined organisms and real benefits, not on category-level hype 4.
That matters in skin discussions because a label that sounds microbiome-aware is still not enough.
The real questions are:
If that sounds familiar, it should. It is the same logic that sits behind our guide to how probiotic selection is evolving: better probiotic decisions are getting more specific, not more magical.
The gut-skin axis gets taken seriously because both the gut and the skin are barrier organs with heavy immune-system involvement. Reviews of the field describe immune-system cross-talk as one of the most credible bridges between intestinal dysbiosis and downstream skin inflammation 5.
This is one reason the gut-skin axis is much more relevant to inflammatory skin conditions than to cosmetic outcomes. Immune tone, tolerance, and inflammatory patterning belong to acne, eczema, psoriasis, and rosacea conversations. They do not automatically belong to anti-aging marketing.
The second major lane is metabolites.
Short-chain fatty acids and other microbial products are often discussed as potential links between diet, gut ecology, and skin-relevant immune signaling 6.
This does not mean one fiber supplement or one probiotic guarantees better skin. It does mean microbiome-sensitive dietary patterns may matter more than readers realize when the question is whole-body inflammatory tone rather than a single cosmetic outcome.
If you want the intervention layer under that idea, use probiotic strains for IBS only for strain-specific logic and use polyphenols and the gut microbiome for the broader mechanism shelf.
The best framing for probiotics here is simple:
That is exactly why this article belongs as a bridge. It is not a product page. It is a decision and interpretation page.
If one skin condition deserves the most careful probiotic discussion, it is atopic dermatitis.
Recent systematic-review and meta-analytic work suggests that microbial interventions may improve some inflammatory-skin-disease outcomes, with atopic dermatitis showing the strongest practical promise inside that literature 7.
But the confidence ceiling matters.
Another pediatric meta-analysis found mixed findings and no clean one-size-fits-all answer, which is a good reminder that strain choice, population, age group, and trial design all influence the result 8.
The fair translation is:
That last point matters because the American Academy of Dermatology's guidance still centers established eczema management, and in pediatric prevention it conditionally recommends against probiotic supplementation for preventing atopic dermatitis 9.
Acne often appears in gut-skin or gut-brain-skin discussions because it is an inflammatory condition affected by hormones, stress, barrier factors, microbial activity, and immune signaling. That makes it mechanistically interesting.
What it does not do is move probiotics into the center of acne standard care.
The AAD acne guideline still emphasizes established topical and systemic therapies such as benzoyl peroxide, retinoids, topical antibiotics, spironolactone, and isotretinoin rather than probiotic-first management 10.
So the cleanest reader takeaway is:
Psoriasis is a chronic multisystem inflammatory disease, which is exactly why it fits the whole-body side of the gut-skin conversation.
Microbiome associations and inflammatory cross-talk make it a reasonable condition to mention in this bridge article, but official psoriasis guidance still centers dermatologist-led therapy and comorbidity-aware management rather than microbiome self-treatment 11.
That makes psoriasis useful here as a reminder that the gut-skin axis is often best treated as an interpretation framework rather than a simple treatment algorithm.
Rosacea and other inflammatory skin conditions do appear in gut-skin reviews, but they should sit in the lower-certainty lane unless the evidence becomes stronger and more clinically direct 12.
This is exactly the kind of place where readers get misled by article sprawl. Once every condition is included, the page starts sounding confident about all of them. That is not what the evidence supports.

The gut-skin axis is most useful when it changes how you read claims, not when it pushes you into random supplement experiments.
Here is the most practical use of the concept:
This is also why the next-step route matters.
Talk to a dermatologist or other qualified clinician first if you are dealing with:
The gut-skin axis does not cancel those priorities.
It may add context. It may shape future adjunctive strategies. It may help you ask sharper questions. But it should not delay diagnosis or turn a serious skin problem into a probiotic shopping project.
Download: Gut-Skin Axis Evidence Ladder and Gut-Skin Axis Clinic Discussion Checklist if you want a one-page summary before your next appointment or before trying another microbiome product.

The gut-skin axis is worth understanding because it offers a serious way to connect gut microbes, barrier function, metabolites, immune signaling, and skin inflammation. It gives readers a better map for interpreting microbiome claims across eczema, acne, psoriasis, and related conditions.
The important discipline is keeping the page in the right lane.
This is not a beauty article. It is not a wrinkle article. It is not a probiotic miracle article.
It is a bridge article.
Use it when you need a better explanation of why skin and gut discussions keep overlapping. Use it to read probiotic claims more carefully. And use it to stay grounded enough to keep standard care, diagnosis, and condition-specific treatment at the center.
This article is for informational purposes only and is not intended as medical advice. Please consult a qualified healthcare provider or dermatologist for diagnosis and treatment of any skin or gastrointestinal condition.
Xam Riche is a gut health solopreneur and founder of YourFitNature, dedicated to helping people navigate digestive wellness through evidence-based information and personal experience. After years of struggling with IBS and bloating, Xam discovered the transformative power of the low FODMAP diet and now shares practical, science-backed guidance to help others find relief. While not a medical professional, Xam combines extensive research with lived experience to create accessible, empowering resources for the gut health community. Learn more about our mission
As an affiliate, we may earn from qualifying purchases.
Showing 10 of 127