
By Xam Riche on April 23, 2026 • 15 min read
This article is for informational and educational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional before using microbiome or supplement content to make treatment decisions.
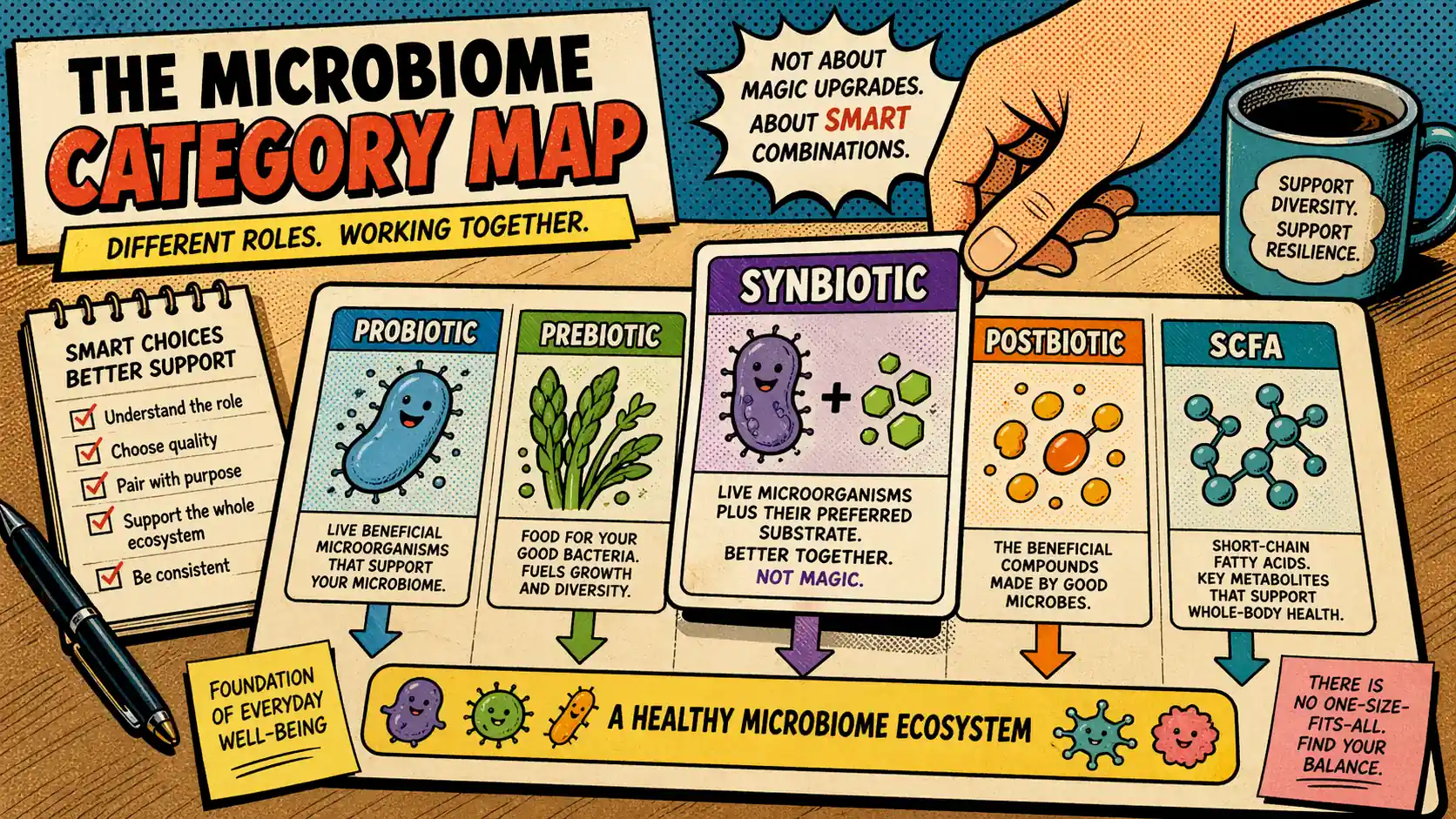
You understood probiotics. Then you learned prebiotics. Now the bottle says synbiotic, another article says postbiotic, and a third explainer talks about SCFAs. At some point, the words stop helping and start selling. Here is the truth: synbiotics can be useful, but a combo formula is not automatically smarter. What matters is the live microbe, the substrate, the dose, the evidence, and whether your gut tolerates the combination.
Short answer: probiotics, prebiotics, synbiotics, postbiotics, and SCFAs are related, but they are not interchangeable. A synbiotic is not just a fancier probiotic. It is a specific mixture of live microorganisms and substrate that should have evidence for a host benefit 1.
This page is for you if you are comparing gut-health labels and want a clear category map before you buy another product or start another trial.
Use a different page first if your real question is already narrower. For strain-level IBS support, use strain-specific probiotic evidence for IBS. For substrate tolerance, use what prebiotic fiber can and cannot do. If your confusion is still just the simplest side-by-side of probiotic vs prebiotic, start there before you move up into the bigger category map. For inactivated microbial products, use postbiotics and what they are not. If the reason you are comparing these categories is a recent antibiotic course, start with antibiotic-induced gut dysbiosis. If the product claim is specifically about sperm health, testosterone, or men's fertility markers, use male fertility-focused probiotic evidence instead of treating it as a generic gut-health category question.
Start with the map.
| Category | What it is | What to ask before trusting the claim |
|---|---|---|
| Probiotic | a live microorganism with evidence for a health benefit | Which strain, dose, population, and outcome were studied? |
| Prebiotic | a substrate selectively used by host microorganisms in a way that benefits health | Which ingredient, dose, and tolerance pattern fit? |
| Synbiotic | a mixture of live microorganisms and substrate that benefits the host | What live microbe, what substrate, and what outcome were tested? |
| Postbiotic | a preparation of inanimate microorganisms and/or components that benefits the host | Which preparation and benefit were demonstrated? |
| SCFA | a microbial metabolite such as acetate, propionate, or butyrate | Is this explaining a mechanism rather than proving a product claim? |
That table is the whole article in miniature.
The mistake is treating all these words as different flavors of the same promise. They sit in the same microbiome conversation, but they point to different things: a live organism, a substrate, a mixture, an inanimate microbial preparation, or a metabolite.
ISAPP's consensus definitions are useful because they make the boundaries clearer instead of louder 2. The goal is not to memorize jargon. The goal is to stop a label from turning five different ideas into one vague gut-health promise.
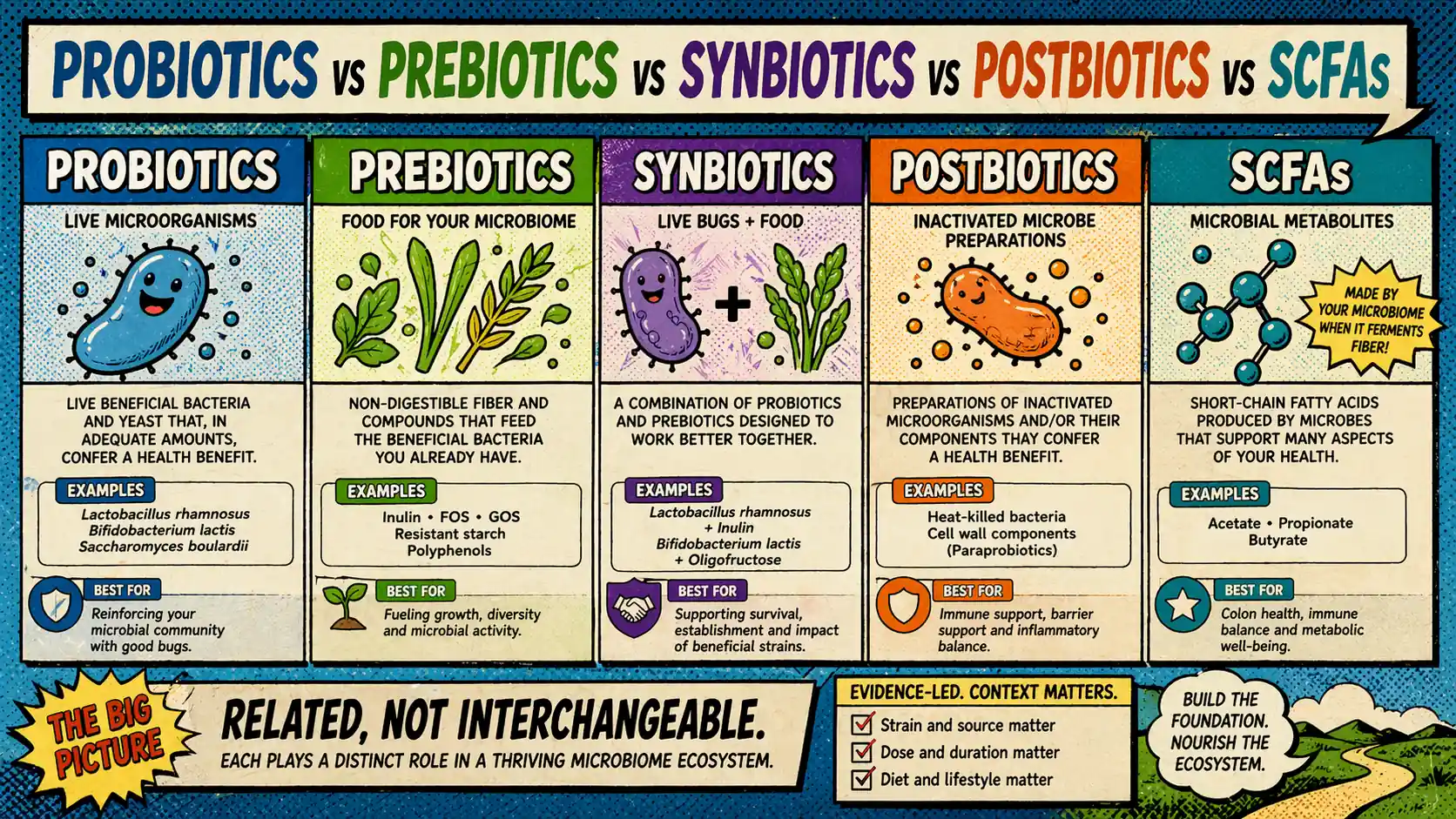
Probiotics are live microorganisms that confer a health benefit when given in adequate amounts. That definition is familiar, but it is only the first filter 3.
The next filter is the one that matters in real life: which strain?
Generic species names and broad "digestive balance" claims are not enough. The evidence for live microbial products depends on the strain, dose, population, and outcome. This is why a probiotic that has data for one symptom or population should not be casually stretched into a universal gut-health claim.
That matters for IBS especially. Guidelines and consumer-facing summaries are cautious because the research is heterogeneous and product-specific 4 5.
Bottom line: "contains probiotics" is not a decision.
The better question is:
If your main question is IBS-D, IBS-C, bloating, or abdominal pain, this page is only the map. The action route is probiotics for IBS strains. If your question has moved beyond category labels and into how strain, formulation, and personalization claims should change the selection itself, use how probiotic selection is evolving.
Prebiotics are not just "fiber with better marketing."
The ISAPP prebiotic definition describes a substrate selectively used by host microorganisms in a way that confers a health benefit 6. That is narrower than the way most labels use the word.
Common prebiotic ingredients include inulin, fructooligosaccharides, often called FOS, galactooligosaccharides, often called GOS, and some resistant starches. These can be useful in the right context.
They can also be the part that makes a "gut-friendly" product feel awful.
That is not a contradiction. A fermentable substrate can be microbiome-relevant and still trigger gas, fullness, or bloating in a sensitive gut. Monash University's low FODMAP materials are relevant here because fructans and GOS sit inside the same broader symptom-management conversation for IBS-prone readers 7.
Here is the practical rule: if inulin, FOS, GOS, or chicory root fiber has already made you bloated, treat that as useful data.
It does not mean prebiotics are bad.
It means the substrate has to fit the person, the dose, and the goal. For the deeper substrate decision, use prebiotic fiber and what it may help.
Synbiotics are where the category map gets more interesting.
ISAPP defines a synbiotic as a mixture comprising live microorganisms and substrate or substrates selectively used by host microorganisms that confers a health benefit 8.
In plain English: a synbiotic combines a live microbial side with a substrate side. But that does not mean any random probiotic plus any random prebiotic deserves a strong claim.
There are two main types.
A complementary synbiotic combines components that each have their own rationale. The probiotic and the prebiotic do not have to prove that they are working as a tightly matched pair. Each part should still make sense for the intended benefit.
The common consumer version looks like this:
The useful question is not "does it combine both?"
The useful question is "does each part fit the goal, and has the mixture been studied for the claim?"
A synergistic synbiotic is more specific. The substrate is selected to be used by the co-administered live microbe. This is a stronger formulation idea, but it also needs more specific evidence.
That is where marketing often gets ahead of the science. A label can imply perfect pairing without showing that the strain, substrate, dose, and outcome were actually tested together.
If constipation is the reason you care about this category, route to synbiotics for constipation-specific decisions. That page goes deeper on bowel frequency, stool pattern, and trial structure.
Two more terms keep showing up beside probiotics, prebiotics, and synbiotics: postbiotics and SCFAs.
They are important, but they are not the same thing.
Postbiotics are preparations of inanimate microorganisms and/or their components that confer a health benefit on the host 9. They are not live probiotics. They are also not just a casual synonym for dead microbes.
SCFAs, short for short-chain fatty acids, are microbial metabolites such as acetate, propionate, and butyrate. They help explain why fermentable substrates and microbial activity matter, but they are not synbiotic products.
The cleanest way to think about it is:
If you need the non-living microbial product category, use postbiotics and what they are not. If you need the metabolite layer, use how SCFAs fit into the microbiome story.
The cleaner question is not "Which biotic is best?"
The cleaner question is "What problem am I actually trying to solve?"
If your question is symptom-specific, start with the symptom. IBS-D, IBS-C, bloating, constipation, and food-trigger sensitivity do not all point to the same next step. A category map helps, but it should not replace the pattern you are seeing in your body.
If your question is product-specific, start with the label. A product that names the strain, substrate, dose, and studied outcome is easier to evaluate than one that hides behind broad microbiome language.
If your question is mechanism-specific, start with the science layer. SCFAs, polyphenols, fiber fermentation, postbiotics, and live microbes all belong to related conversations, but they answer different questions. Mechanism clarity is useful. It just does not automatically tell you which product to take.
Here is the practical sequence:
That order prevents a common mistake: using a scientific term as permission to skip the basics.
For example, a synbiotic may look more complete than a probiotic because it contains both a live microbe and a substrate. But if your main problem is violent bloating from inulin-heavy products, the prebiotic side of the formula may be the first thing to question. If your main problem is strain-specific IBS support, the extra substrate may be less important than whether the strain has relevant data. And if your main problem is simply that all the terms are blending together, the category map is the right starting point.
Sometimes a synbiotic may make more sense than a probiotic alone.
But only under specific conditions.
A synbiotic is more plausible when:
It is less plausible when:
This matters because the added prebiotic is often the selling point. In a sensitive gut, it may also be the part that causes gas, fullness, or bloating.
NCCIH and NIH ODS both emphasize that probiotic safety and usefulness depend on the product and the person, especially for people who are immunocompromised, critically ill, or managing serious medical conditions 10 11. For a serious-condition example, the colorectal cancer microbiome-claim guide separates probiotic supportive-care research from cancer screening, diagnosis, and treatment decisions.
So no, a synbiotic is not automatically better.
It is only a better fit when the formula matches the goal and your gut can handle the substrate.
The fastest way to stop guessing is to make the label answer better questions.
Ask:

[!TIP] Download: Synbiotic Label Checklist Use it before buying another combo product so you can separate a real synbiotic claim from broad gut-health marketing.
The right next read depends on the question you are actually trying to answer.
[!TIP] Download: Biotic Category Map Keep it nearby when probiotics, prebiotics, synbiotics, postbiotics, and SCFAs start blending together.
Sometimes the problem is not that you picked the wrong category.
Sometimes the real issue is that symptoms need broader sorting.
Persistent or worsening bloating, severe pain, repeated vomiting, bleeding or black stools, unexplained weight loss, or inability to pass stool or gas deserve medical review rather than another round of label comparison 12 13.
This is especially important if every product sounds logical but your body keeps reacting badly. That pattern may need symptom-first troubleshooting, not another microbiome label.
For that route, use when another gut-health product is not the answer.
Synbiotics, probiotics, and prebiotics are worth understanding. They are just not worth blurring together.
Here is the cleanest way to use the category map:
If you want the broader science shelf behind food-to-microbe interactions, start with the broader microbiome mechanism shelf. If your next question is constipation-specific, go to synbiotics for constipation. If your next question is product category clarity, move across to postbiotics or short-chain fatty acids.
Xam Riche is a gut health solopreneur and founder of YourFitNature, dedicated to helping people navigate digestive wellness through evidence-based information and personal experience. After years of struggling with IBS and bloating, Xam discovered the transformative power of the low FODMAP diet and now shares practical, science-backed guidance to help others find relief. While not a medical professional, Xam combines extensive research with lived experience to create accessible, empowering resources for the gut health community. Learn more about our mission
As an affiliate, we may earn from qualifying purchases.
Showing 10 of 152