
By Xam Riche on May 1, 2026 • 15 min read
This article is for informational and educational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional before using microbiome or supplement content to make diagnosis or treatment decisions.
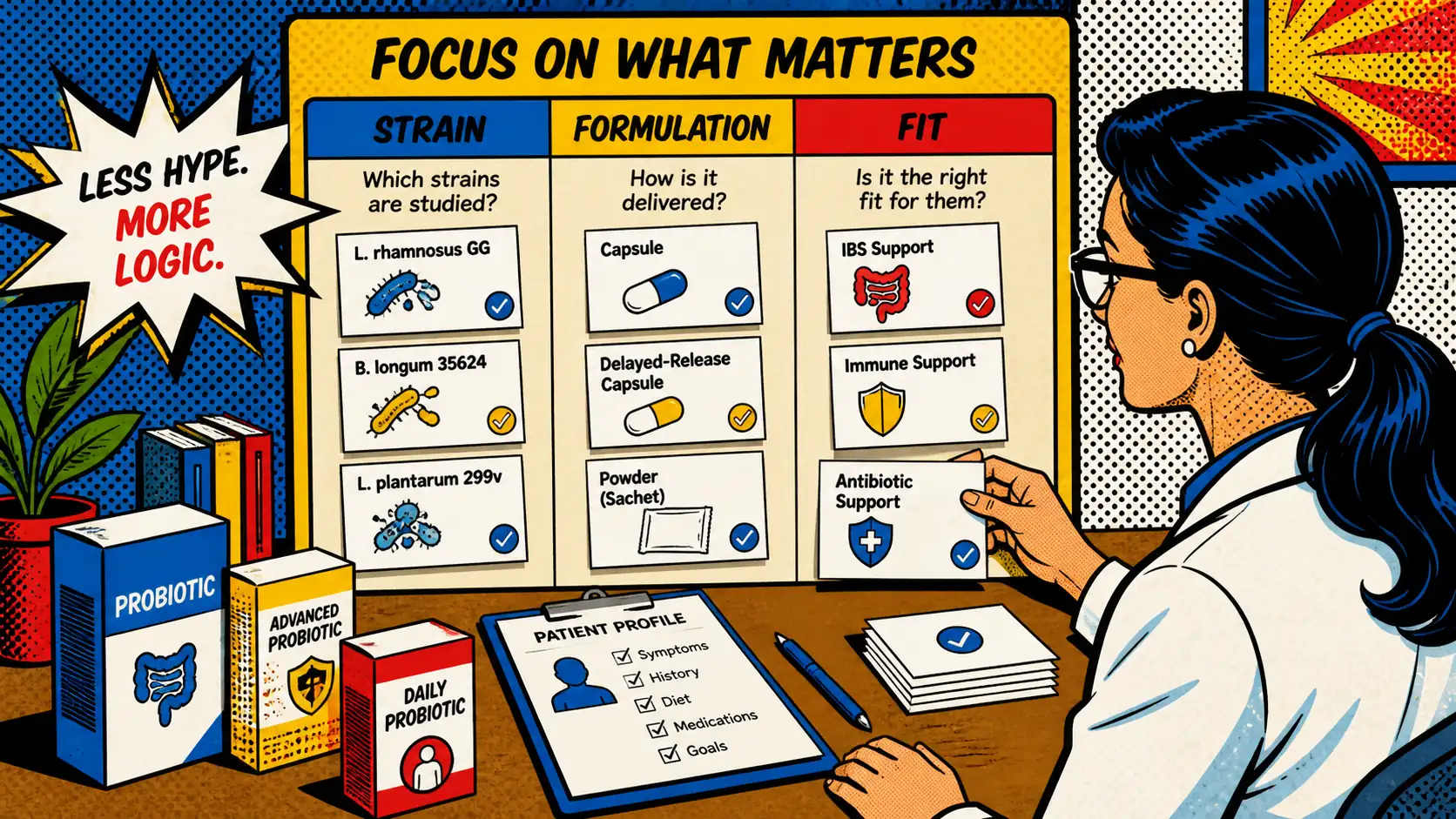
The probiotic shelf used to feel confusing because every bottle sounded the same. Now it feels confusing because they all sound different. One pushes CFU count. Another highlights strain codes. Another says synbiotic. Another says microbiome-based or personalized. That sounds more advanced, but not necessarily more useful. What most readers need now is not another louder promise. They need a better filter for what probiotic selection is actually becoming.
Short answer: probiotic selection is evolving toward more specific questions about strain, studied outcome, dose, formulation, and patient fit. That is real progress. It is not the same as saying current consumer stool testing or next-generation branding can reliably personalize the answer for everyone 1 2.
This page is for you if you already understand the basic probiotic idea and now want to know how to choose more intelligently without falling for hype.
Use a different page first if your main question is already narrower. If you need the broader category parent, start with synbiotics, probiotics, and prebiotics. If your real question is symptom-specific, move straight to probiotic strains for IBS. If the bigger selection logic helps but your next question is specifically IBS-D, use what evidence matters when choosing probiotics for IBS-D. If the claim is about men's fertility or hormone-adjacent benefits rather than gut symptoms, use male fertility-focused probiotic evidence so that niche claim does not get folded into general probiotic selection.
For years, many readers were taught three simple probiotic shortcuts:
Those shortcuts are now too crude.
NIH's Office of Dietary Supplements defines probiotics as live microorganisms that provide health benefits when taken in sufficient amounts and notes that labels should identify the organism clearly enough to include genus, species, and strain when relevant 3. The World Gastroenterology Organisation uses the same formal definition and frames probiotic effects as product-specific rather than automatically category-wide 4.
That changes the consumer problem completely.
The question is no longer just, "Should I take a probiotic?" The better question is, "Which organism or formulation was studied for the outcome I care about, and does this product actually resemble that evidence?"
This is why the old probiotic shelf logic breaks down:
If you have already solved the first category question of probiotic vs prebiotic, this article is the next layer. It is about how the decision itself is getting more specific.
The most important change in probiotic thinking is that the field keeps moving away from category-level language and toward strain-specific and outcome-specific thinking.
At the category level, two products can both say Lactobacillus or Bifidobacterium and still be very different practical choices. The strain code is not a cosmetic add-on. It is often the part that connects the label to the actual study population and measured outcome.
That matters most when people move from "gut health curiosity" to actual symptom decisions.
In IBS, for example, the American Gastroenterological Association does not recommend treating probiotics as a broad, reliable category solution because the evidence is too heterogeneous 5. A 2023 meta-analysis reached a similar conclusion in a more nuanced way: some probiotics may help IBS, but differences in species, strains, mixtures, and endpoints make simple category-wide recommendations hard to defend 6.
That is not a dismissal of probiotics.
It is a correction: better selection starts by getting narrower, not by getting louder.
A strain studied for one outcome should not be stretched casually into another. If the question is IBS symptom fit, the next route is probiotic strains for IBS, not a generic "gut wellness" blend. If the question is whether a probiotic claim is being used to imply bigger heart-health benefits than the evidence supports, use the gut-heart axis shelf to separate microbiome mechanism from cardiometabolic overclaim. If the same kind of claim is being stretched into skin-health certainty, use the gut-skin axis explainer to separate inflammatory-skin-condition evidence from cosmetic probiotic hype. If probiotic or microbiome language is being stretched into colorectal cancer care, use this stricter cancer-claim boundary guide before treating supportive-care research as treatment advice.
The 2021 strain-specific IBS meta-analysis is especially useful here because it argues for judging probiotic effects by the strain or mixture and the measured outcome, not just by the presence of a probiotic label 7.
The newer reading order is:
That is a very different consumer behavior from just comparing bottle size or billions of CFUs.

Strain specificity matters, but it is not the whole story. Selection quality is also becoming more formulation-aware.
NIH ODS points out that higher CFU counts do not automatically produce greater benefits and that labels differ in whether they report counts at manufacture or through expiry 8. That means "billions of CFUs" is not useless information, but it is poor as a standalone shortcut.
The better question is whether the product's dose, viability, storage needs, and delivery format make sense for the studied use. A strain with plausible data can still be a poor real-world pick if the formulation does not preserve what the evidence assumed.
The shelf has also become more confusing because products increasingly mix live microbes with prebiotic substrates. Sometimes that is reasonable. Sometimes it adds a useful complementary layer. Sometimes it just adds another way for the product to be a poor fit.
That is why the question "Is a synbiotic better?" is weaker than the question "Does the organism, substrate, dose, and purpose actually fit this use case?" If you need the category parent for that distinction, go to synbiotics, probiotics, and prebiotics. If you still need the simpler binary first, use probiotic vs prebiotic.
This is the part many readers learn the hard way. Added inulin, FOS, or other fermentable ingredients can change tolerance. A product may sound smarter on paper because it combines more elements, but that does not make it a better match for a gut that already reacts badly to fermentation-heavy add-ins.
This is one reason selection is evolving away from "most complete formula wins" and toward "does this formulation match the job?" If constipation is the real decision context and you are weighing combo products, use synbiotics for constipation instead of assuming all add-ins are harmless upgrades.
The next change is more practical than technical: probiotic choice is becoming more patient-fit oriented.
The same product logic does not apply equally across:
That sounds obvious, but it is exactly where shelf decisions still go wrong.
If the real question is symptom fit, go down to probiotic strains for IBS. If the context is recovery after antibiotics, use antibiotic-induced gut dysbiosis so the decision lives inside the right clinical frame.
One person's tolerable formula can be another person's trigger. If previous trials worsened gas, fullness, urgency, or bloating, that matters. It does not prove probiotics are useless. It means the product, context, or the entire problem framing may have been a mismatch.
If "healthy" products keep making you feel worse, the next shelf is often not a fancier probiotic. It may be why you still feel bloated after eating healthy foods.
This is where personalization starts to sound reasonable. Host context matters. Background diet matters. Tolerance matters. The resident microbiome matters. But those truths should improve the quality of your questions, not convince you that any brand can now promise your exact answer.
This is the section where the hype usually accelerates.
Personalization sounds plausible because the biology is not uniform. A landmark 2016 study found that stable engraftment of one Bifidobacterium longum strain depended on individualized features of the resident microbiome and that colonization was often transient 9. A later review on colonization mechanisms argues that persistence and fit are influenced by strain behavior, diet, immune interactions, and the background microbiome 10.
So yes, one person's response can differ meaningfully from another person's. That is real.
Where the hype outruns the evidence is the jump from "host context matters" to "this stool test or quiz can tell you your best probiotic with confidence."
The field is moving toward more personalized control of gut bacterial communities, but even research-facing overviews describe that as an active development challenge rather than as a solved everyday consumer tool 11.
That is the boundary readers need.
Personalization is:
Personalization is not yet:
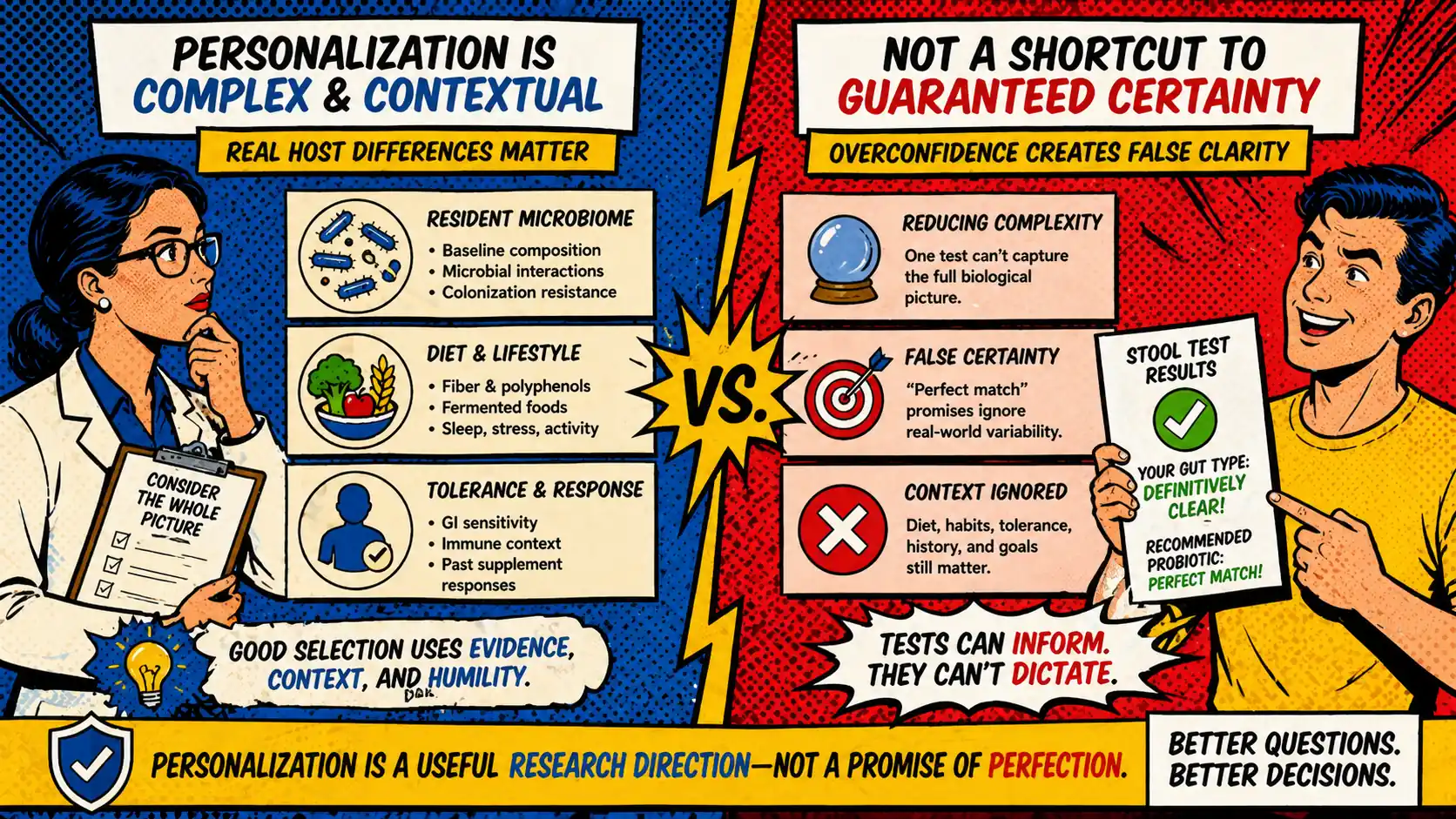
The practical move is not to reject personalization language entirely. It is to translate it into cleaner questions:
That is how personalization becomes useful without becoming magical.
Another reason probiotic selection feels like it is evolving is the emergence of so-called next-generation probiotics.
This term usually refers to microbial candidates outside the older consumer-familiar shelf, often chosen because of newer mechanistic or translational research rather than because they have decades of routine retail history 12.
That is scientifically interesting.
It is also easy to misuse in marketing.
The cleanest way to think about next-generation probiotics is:
Akkermansia muciniphila is the standard example here. It has compelling research interest and human proof-of-concept metabolic data, but that still does not make it a routine, symptom-agnostic answer for everyday gut complaints 13.
If you see next-generation language blended with non-living microbial claims, pause and compare it with the adjacent postbiotics shelf rather than assuming everything new belongs under one upgraded umbrella. And if you want the broader mechanism background behind why microbial interventions keep expanding, the parent science route is polyphenols and the gut microbiome.
The simplest anti-hype framework is this:
Download: Probiotic Selection Checklist
Use this one-page reference to check strain, outcome, formulation, and fit before trusting another probiotic promise.
Download: Probiotic Claim Red Flags Map
Use this quick sheet to spot CFU-only marketing, fuzzy personalization claims, and category drift before you spend more money.
If every probiotic seems to make things worse, the answer is not always a more advanced probiotic.
Persistent pain, bleeding, fever, vomiting, significant weight loss, or rapidly changing symptoms need evaluation rather than endless product rotation. Even in less dramatic cases, repeated failure can be a clue that the main problem is not "the wrong bottle" but the wrong frame. If the whole system of gut-health products keeps backfiring, step sideways into why you still feel bloated after eating healthy foods instead of assuming the next supplement tier will finally solve it.
If you are already combining probiotics with digestive enzymes, peppermint oil, fiber, magnesium, ginger, prebiotics, or fermented-food experiments, stop shopping and use the supplement stack audit for IBS. The problem may be too many moving parts, not a missing next-generation product.
| Situation | Best next read | Why |
|---|---|---|
| You need a strain-level IBS decision | Probiotics for IBS strains guide | It maps named strains to diarrhea, constipation, bloating, pain, and overall IBS severity. |
| You are unsure whether the category is probiotic, prebiotic, or synbiotic | Synbiotics, probiotics, and prebiotics | It separates live microbes from substrates and combination products. |
| You are using a stool or microbiome report to pick a product | Stool and microbiome tests for IBS | It explains why consumer microbiome outputs are not probiotic prescriptions. |
| You are already stacking gut-health tools | Supplement stack audit for IBS | It helps test one variable at a time before the routine becomes unreadable. |
| Symptoms are persistent, changing, or medically complex | Doctor visit prep for IBS next steps | It helps organize symptom patterns, medications, supplements, and questions for a clinician. |
Probiotic selection is evolving in a useful direction.
It is becoming more specific about strain, studied outcome, formulation, and host context. That is better than the old "more CFUs and more promises" model. But it still does not justify pretending that probiotic choice has already become fully personalized certainty.
Use the new logic in this order:
If your next question is narrower, route out cleanly:
Better probiotic selection means clearer strain, outcome, formulation, and fit. It does not mean microbiome tests, personalization language, or a more advanced label can remove uncertainty. If the routine is getting crowded, simplify before you escalate.
Xam Riche is a gut health solopreneur and founder of YourFitNature, dedicated to helping people navigate digestive wellness through evidence-based information and personal experience. After years of struggling with IBS and bloating, Xam discovered the transformative power of the low FODMAP diet and now shares practical, science-backed guidance to help others find relief. While not a medical professional, Xam combines extensive research with lived experience to create accessible, empowering resources for the gut health community. Learn more about our mission
As an affiliate, we may earn from qualifying purchases.
Showing 10 of 127