
By Xam Riche on May 1, 2026 • 13 min read
This article is for informational and educational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional before using supplement or microbiome content to make diagnosis or treatment decisions.
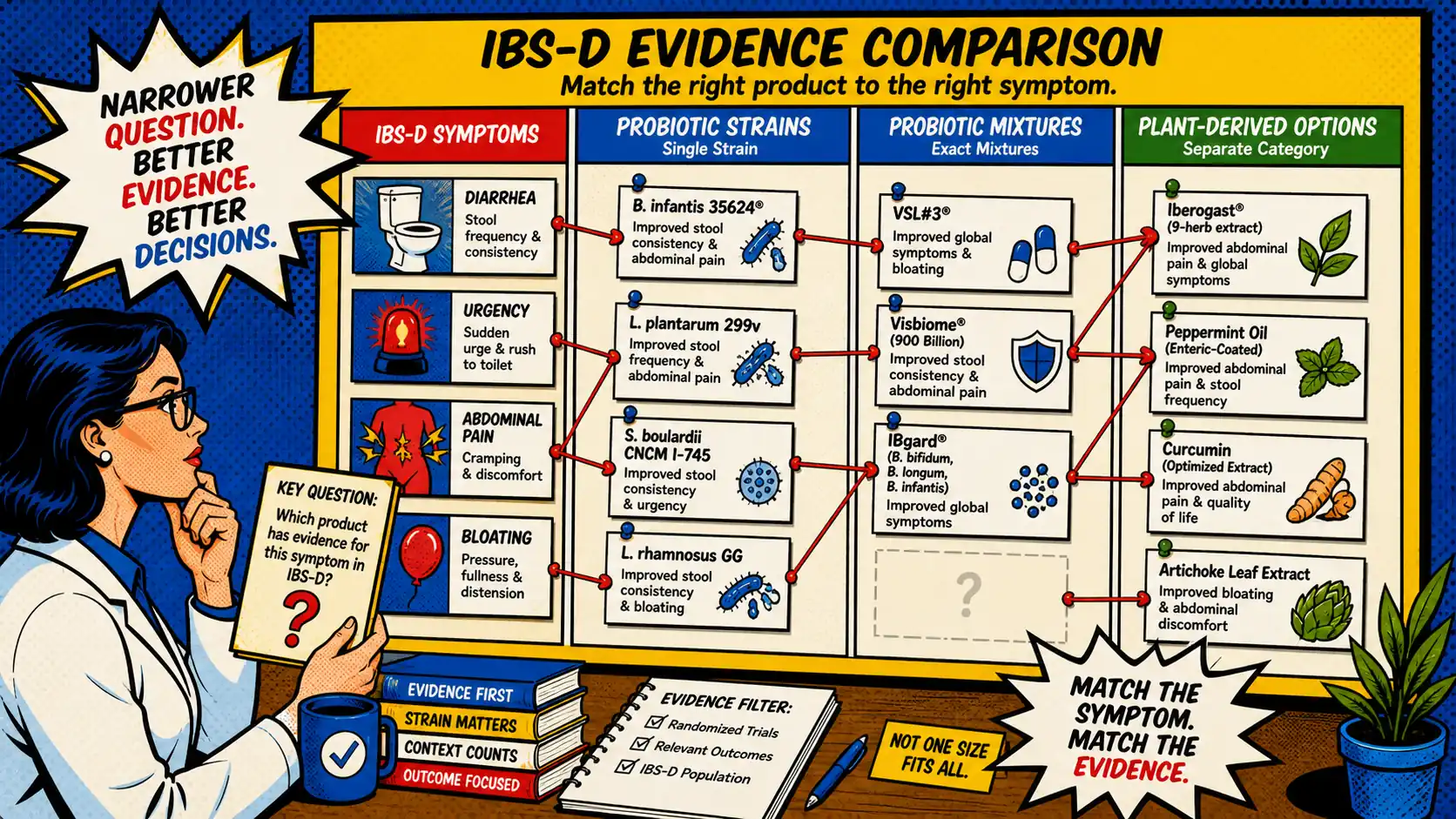
IBS-D supplement shopping gets confusing fast because the shelf no longer holds just probiotics. It also holds synbiotics, gut-support blends, plant-derived formulas, and product pages that promise "natural IBS-D relief" without making it clear whether they are talking about stool consistency, urgency, pain, or bloating. What most readers need is not another louder recommendation. They need a better evidence filter.
Short answer: the best IBS-D product decision usually starts by getting narrower. Match the intervention to the symptom outcome first, then check whether the exact product class, exact formulation, and exact study signal actually line up. That matters more than broad category language like "probiotic," "natural," or "gut support" 1 2.
This page is for you if your question is not just "which strain helps IBS?" but "how do I judge whether any IBS-D product claim is strong enough to trust?"
Use a different page first if your real question is already more specific. If you want the parent strain shelf, go to probiotic strains for IBS. If your question is broader than IBS-D and you are trying to understand the changing probiotic shelf itself, use how probiotic selection is evolving.
Many readers assume the main task is finding the strongest product in one simple category. IBS-D research does not work that cleanly.
The American College of Gastroenterology recommends against probiotics for global IBS symptoms because the overall literature is highly heterogeneous and the evidence quality remains low 3. The American Gastroenterological Association takes a similarly cautious position, noting that broad class-level support is not strong enough for IBS 4.
That does not mean every probiotic signal is equally useless.
It means category-level reasoning is weak. You should not trust a bottle simply because it says probiotic, high potency, or digestive balance. The evidence gets more meaningful when the intervention is exact and the symptom outcome is exact.
This is also where category confusion causes bad comparisons. A plant-derived IBS-D product is not automatically a probiotic and should not be treated as if it belongs in the same evidence lane. If a label is built around a plant-derived barrier-support formulation or a separate antisecretory compound, that is a different intervention question, not just a more "natural" probiotic upgrade 5.
So the right question is not, "What is the best probiotic for IBS-D?"
The better question is, "Which exact intervention was studied for the IBS-D outcome I care about, and how strong is that signal compared with the marketing around it?"
The biggest shopping mistake is treating IBS-D like one single endpoint.
It is not.
IBS-D readers may be mainly trying to change:
Those outcomes overlap, but they are not interchangeable. A product studied for one can sound much more proven than it really is if the label quietly drifts into broader language.
The newer IBS probiotic literature is useful here because it keeps pushing toward outcome-specific thinking. A 2021 systematic review and meta-analysis argued that probiotic efficacy should be judged at the strain-specific or mixture-specific level and by the exact IBS outcome being measured, not by class-wide probiotic identity alone 6.
The 2023 network meta-analysis makes the same lesson even more practical for IBS-D. Some probiotics ranked better for bowel movement frequency, while others showed stronger signal for stool form or other endpoints. The point is not that one bottle is universally "best." The point is that the evidence changes when the endpoint changes 7.
That matters because IBS-D product pages often blur:
If your main question is exact strain selection for IBS-D, use the parent page on probiotic strains for IBS. That page is the better shelf for named organisms and symptom matching. If diarrhea and urgency are still the center of the decision, it also helps to anchor the rest of the plan in low-FODMAP changes for IBS-D so the supplement decision is not being asked to do all the work alone.
The rule to keep is simple:
The closer the measured trial outcome is to your dominant symptom, the more useful the evidence becomes.

Once the symptom outcome is clear, the next question is whether the product identity is specific enough to mean anything.
If a product does not clearly identify the strain or at least the exact studied mixture, your ability to map it onto the IBS-D literature gets much weaker. This is the same core rule explained in how probiotic selection is evolving: selection quality improves when the intervention becomes more specific, not more glamorous.
That is why a generic "contains Lactobacillus and Bifidobacterium" claim is not enough. Even when the broad category seems relevant, the actual evidence lives at the strain or exact formulation level 8.
This is the biggest category error readers need to avoid.
Crofelemer is not a probiotic strain. Xyloglucan-based formulations are not probiotic strains. They may still matter in IBS-D, but they belong to a different mechanism lane.
The Frontiers review on IBS-D pharmacologic targets is useful here because it places probiotics and plant-derived products beside each other as possible non-pharmacologic or adjunctive options while still keeping them distinct 9. That is the right way to frame them.
If a product is built around:
That matters because these products should not be compared as if they are just different flavors of the same intervention.
Words like natural, plant-based, or gentle can make categories blur. They can also hide the more important question of whether the exact intervention was studied for the exact IBS-D problem you have.
If you are still separating the basic taxonomy shelf, use probiotic vs prebiotic or synbiotics, probiotics, and prebiotics before you let lifestyle language substitute for intervention identity.
Once you know the outcome and the intervention identity, the next issue is study strength.
Guidelines stay cautious because the probiotic literature in IBS is crowded, heterogeneous, and often difficult to generalize. Different studies use different organisms, mixtures, doses, durations, and endpoints. Some show signal. Some do not. Some use outcomes that are too broad to help with a narrow shopping decision.
That is why the class-wide recommendation stays weak even when individual signals exist 10 11.
For a reader actually comparing products, stronger probiotic evidence usually looks like this:
That is a much better standard than trusting CFU count, marketing adjectives, or "doctor recommended" language.
The plant-derived lane is even more important to read cautiously because the evidence base is smaller and more formulation-specific.
For xyloglucan plus pea protein, tannins, and xylo-oligosaccharides, there is a promising signal around diarrhea control, pain, and broader IBS-D symptom management in formulation-specific studies, including a long-term open-label observational study and a more recent translational evaluation 12 13.
That is interesting. It is not the same thing as saying the whole plant-derived product shelf is now strongly established.
Crofelemer is even more nuanced. In a randomized trial in women with IBS-D, it did not become a universal answer across all outcomes. The more interesting signal was around pain and discomfort outcomes in women, not a clean, all-purpose IBS-D win 14.
This is exactly why evidence sorting matters.
If a product page stretches a subgroup or outcome-specific signal into a broad "great for IBS-D" promise, the marketing has outrun the evidence.
Even a reasonable active intervention can be a poor real-world fit if the rest of the formula is wrong for you.
Some readers do badly not because the whole intervention idea is useless, but because the commercial product adds fermentable ingredients, excipients, or combo elements that shift the tolerance picture.
This matters especially when the product is sold as a smarter combined formula. If added prebiotic fibers or combo ingredients have repeatedly worsened bloating, gas, or fullness, that is real decision data. It is not something to ignore just because the label sounds advanced.
If you need the broader formulation shelf first, use prebiotic fiber and when it can backfire and synbiotics, probiotics, and prebiotics.
Once a product adds prebiotics or multiple intervention layers, the reader is no longer judging just a probiotic decision. They are judging a second formulation decision on top of the strain question.
That is why "more complete" is not automatically better. It may be better. It may also make the product harder to interpret and less tolerable.
If your gut keeps reacting badly to supposedly healthy products, do not treat that as proof that you are doing something wrong. Treat it as evidence that the frame may be off.
If every "gut support" experiment seems to increase bloating, urgency, or abdominal chaos, step sideways into why you still feel bloated after eating healthy foods instead of assuming the answer is still one shelf higher.
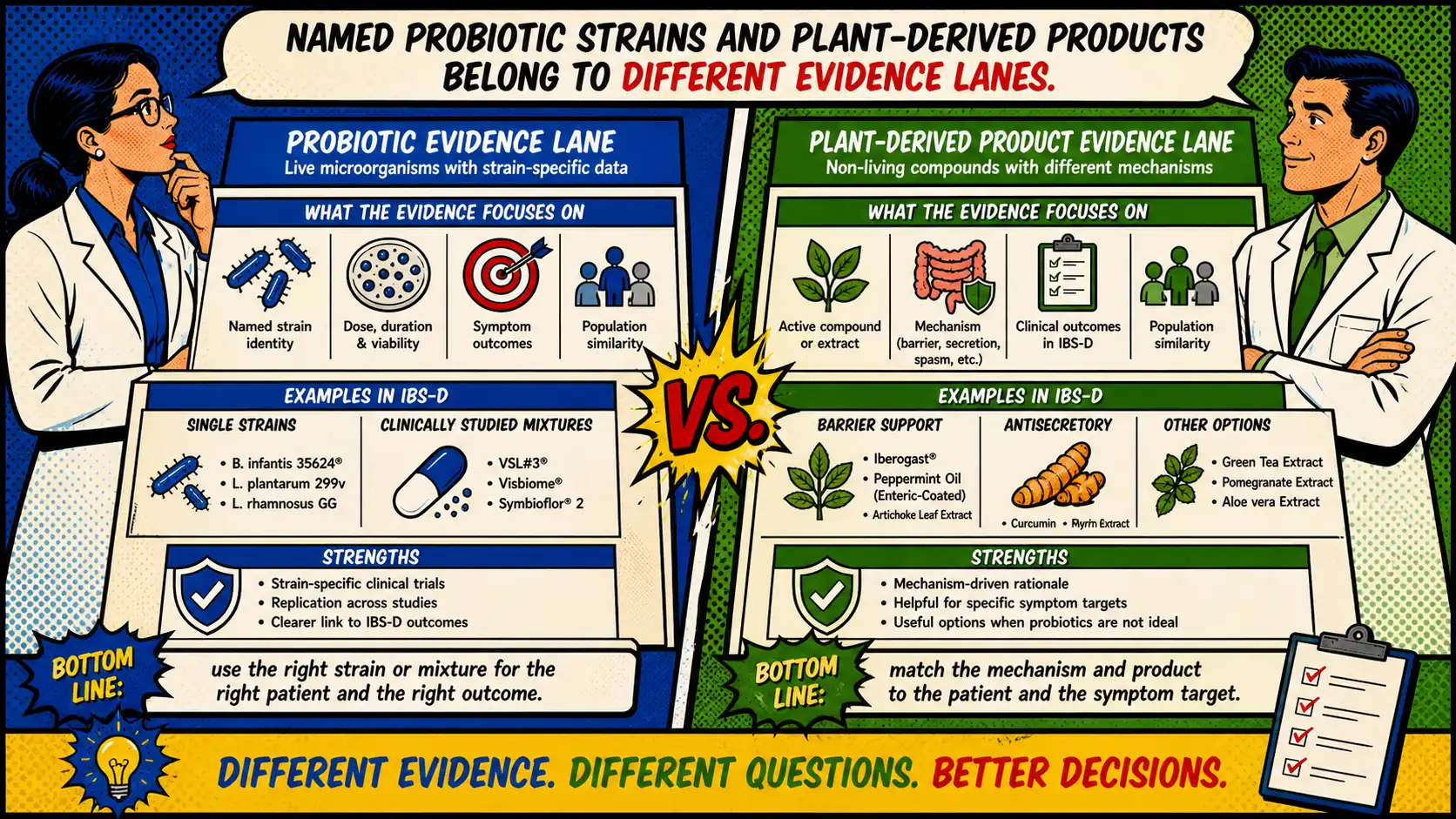
Plant-derived products deserve a place in the discussion, but only with clear boundaries.
The cleanest way to think about them is:
For the xyloglucan combination lane, the appeal is not microbiome glamour. It is barrier and symptom-support logic. The current signal comes from formulation-specific observational and translational work suggesting improvement in stool consistency and broader symptom burden in some IBS-D settings, but the reader should still treat the evidence as formulation-specific rather than as a general proof that plant-derived products are broadly superior 15 16.
For crofelemer, the main lesson is even narrower. It is worth knowing because it shows how one plant-derived compound can have outcome-specific or subgroup signal without becoming a universal IBS-D recommendation 17.
If your main goal is comparing non-pharmaceutical symptom tools more broadly, route out to peppermint oil for IBS or the broader IBS treatment shelf rather than forcing everything into a probiotic framework.
Use this order every time:
Download: IBS-D Probiotic Evidence Filter
Use this one-page checklist to judge outcome match, intervention identity, replication, formulation fit, and warning signs before buying another product.
Download: IBS-D Plant Product vs Probiotic Decision Card
Use this quick card to separate probiotic evidence lanes from separate plant-derived formulation lanes.
Supplements are not the right frame for every IBS-D problem.
Bleeding, fever, weight loss, nighttime diarrhea, significant dehydration, or escalating pain need evaluation rather than more product rotation 18. Even without dramatic red flags, repeated failure can be a clue that the main issue is not "the wrong probiotic" but a larger diagnostic or management problem.
If the product shelf keeps failing you, step back into the bigger treatment and troubleshooting shelves instead of asking every new bottle to solve the same unanswered question.
The strongest IBS-D product decisions usually come from a narrower filter, not a broader supplement category.
Use the evidence in this order:
If your question is now more specific, route out cleanly:
Xam Riche is a gut health solopreneur and founder of YourFitNature, dedicated to helping people navigate digestive wellness through evidence-based information and personal experience. After years of struggling with IBS and bloating, Xam discovered the transformative power of the low FODMAP diet and now shares practical, science-backed guidance to help others find relief. While not a medical professional, Xam combines extensive research with lived experience to create accessible, empowering resources for the gut health community. Learn more about our mission
As an affiliate, we may earn from qualifying purchases.
Showing 10 of 127