
By Xam Riche on March 20, 2026 • 12 min read
This article is for informational and educational purposes only and does not constitute medical advice. Always consult with a registered dietitian, gastroenterologist, or other qualified medical professional before making significant dietary changes.

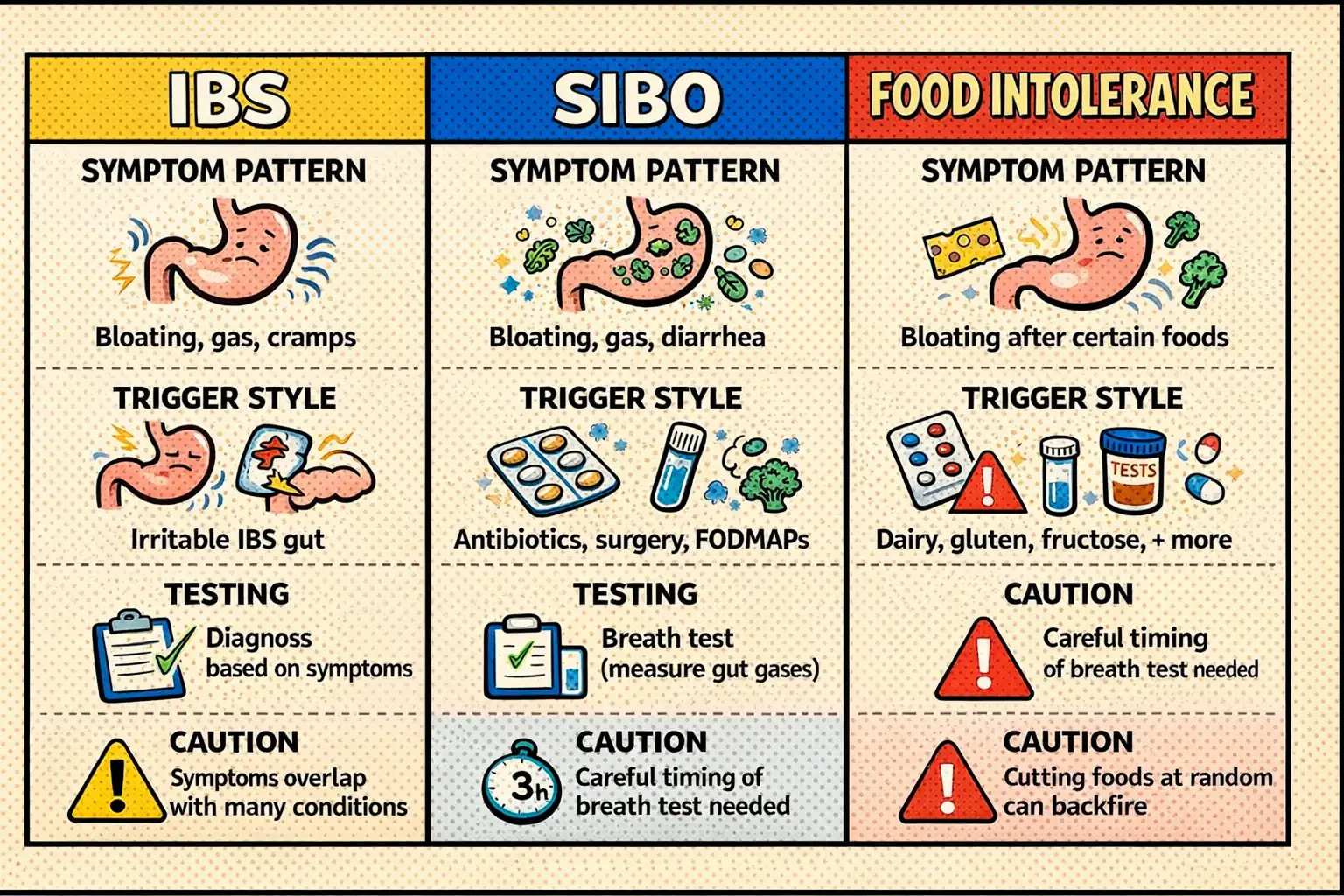
IBS, SIBO, and food intolerance can all show up as bloating, pain, and messy reactions after eating. This guide helps you sort the pattern more clearly so you know whether to think in terms of a broad IBS pattern, a specific food trigger, or a SIBO-style overgrowth question worth discussing with a clinician.
This page is for readers whose main problem is pattern differentiation. The short answer is that IBS usually behaves like a broader chronic bowel-pattern problem, food intolerance behaves more like a repeat narrow trigger with dose effects, and SIBO becomes more plausible when the whole clinical context points toward overgrowth rather than one food alone.
If you already know low FODMAP failed and now need a troubleshooting ladder, move straight to what to do when low FODMAP is not working. If you need the wider symptom-entry map before comparing diagnoses, return to how to reduce bloating.
You eat yogurt and bloat. Another day it happens after garlic sauce. Another day it happens after a meal that should have been safe. That is usually when the internet turns into a diagnostic slot machine.
IBS. SIBO. Lactose intolerance. Fructose intolerance. "Maybe it is all of the above."
The confusion is understandable. These labels overlap enough to make careful people feel reckless and anxious people feel certain. The goal of this article is not to help you diagnose yourself from one table. The goal is to help you recognize the pattern more accurately and decide what next step is reasonable.
If you need the broader troubleshooting ladder after this comparison, use what to do when low FODMAP is not working.
At the symptom level, these three categories share a lot of ground:
NIDDK defines IBS as repeated abdominal pain plus changes in bowel movements, without visible signs of digestive-tract damage or disease 1. ACG lists belly pain, bloating, bowel habit changes, gas, fatigue, and nausea among common SIBO symptoms 2. NIDDK also lists food intolerances such as lactose intolerance, dietary fructose intolerance, and sugar alcohols separately from SIBO and IBS as possible causes of chronic diarrhea 3.
So yes, the overlap is real.
The useful question is not "Which symptom belongs to which label?" It is "What does the pattern over time look like?" If you want the bigger map of bloating causes beyond these three buckets, start with many causes of bloating.
IBS usually looks less like one isolated food drama and more like an ongoing symptom pattern.
NIDDK describes IBS as repeated abdominal pain together with changed bowel movements 4. NICE says IBS should be considered when symptoms such as abdominal pain or discomfort, bloating, and change in bowel habit have been present for at least 6 months, and it gives positive symptom criteria rather than requiring endless open-ended testing 5.
In practical terms, IBS becomes more plausible when:
That is why IBS often feels bigger than a single trigger food. Food still matters, but it is usually part of a larger pattern rather than the whole story.
If you are early in the diet phase of troubleshooting, the best companion here is the low-FODMAP process. And if your symptoms get louder during stressful weeks even when food is unchanged, review how stress can amplify IBS symptoms.
The ACG guideline defines SIBO as excessive bacteria in the small bowel causing gastrointestinal symptoms 6. That definition matters because SIBO is not just "bloating after carbs." It is a symptom picture plus a specific overgrowth question.
The overlap with IBS is still substantial. ACG lists pain, bloating, gas, diarrhea, constipation, and nausea among common SIBO symptoms 7. A systematic review also found higher SIBO prevalence in IBS patients than in controls, though the estimates vary a lot depending on how SIBO is defined and tested 8.
SIBO becomes more plausible when the picture includes a broader fermentation pattern rather than one repeat food alone, especially if there are additional context clues such as motility problems, prior GI surgery, diabetes, opioid use, or another reason small-bowel bacterial overgrowth might be more likely 9.
That does not mean every bloated person probably has SIBO. It means SIBO deserves discussion when the pattern and the clinical context line up.
Testing matters here. ACG says hydrogen breath testing is the most common indirect way to measure excess small-intestinal bacteria 10. The North American Consensus says glucose and lactulose breath tests are the least invasive alternatives for diagnosing SIBO and provides standardized thresholds for interpretation 11. If this sounds like your lane, use the broader SIBO workup and next-step guide.
Food intolerance is usually narrower and more repeatable.
AAAAI says food intolerance happens in the digestive system, often involves difficulty breaking down a food, and may be tolerated in small amounts, unlike food allergy which involves the immune system and can be life-threatening 12. That is a useful distinction because many readers casually say "allergy" when they really mean "digestive trigger."
Food intolerance becomes more plausible when:
Lactose intolerance is the cleanest example. NIDDK says a doctor may diagnose lactose intolerance when breath hydrogen rises and symptoms worsen during lactose breath testing 13. Monash also notes that lactose intolerance is often amount-dependent, with many people tolerating some lactose rather than none 14.
Fructose and sugar alcohol sensitivity can matter too, but the testing story is less straightforward. Monash reports that routine fructose breath testing is not well supported for guiding management in IBS because results are not reproducible enough and do not correlate well with symptoms 15.
That is why food intolerance is best treated as a pattern question first and a test question second.
If your main issue is how to describe narrow triggers in the real world, use food intolerances in restaurants. If the suspicion is more about specific label ingredients than whole-food categories, go to specific ingredient triggers.
Use the table below as a sorting tool, not a diagnosis certificate.
| Feature | IBS | SIBO | Food Intolerance |
|---|---|---|---|
| Typical pattern | chronic symptom syndrome with bowel habit change | GI symptoms plus small-bowel overgrowth suspicion | specific food or carbohydrate trigger pattern |
| Common symptoms | pain, bloating, diarrhea, constipation, urgency | pain, bloating, gas, diarrhea or constipation, nausea | bloating, gas, diarrhea, cramping after specific foods |
| Trigger style | broad and often multi-factorial | broad fermentation-type flares | narrower and more reproducible |
| Diagnosis route | symptom criteria plus limited rule-out tests | clinical context plus breath testing | food-specific history, challenge/elimination, sometimes breath testing |
| Main caution | not just "nothing found" | not every bloated person has it | not the same as food allergy |
[!TIP] Download: Symptom Pattern Comparison Worksheet Use it to track symptom timing, repeat foods, dose effects, bowel-pattern changes, and testing questions before your next appointment.
Yes, and this is where the whole topic gets messy.
Someone can meet IBS criteria and also react strongly to lactose. Someone with a broad IBS-like pattern can also have a narrow sugar-alcohol trigger. And the North American Consensus says SIBO should be excluded before breath testing for carbohydrate malabsorption to avoid false positives 16. In other words, overgrowth can muddy the way carbohydrate testing reads.
That is why three common mistakes keep wasting time:
If you are in the middle of food testing, the best next move is often structured testing instead of guessing. And if you are hoping supplements will somehow solve the whole picture, remember that enzymes are not a universal fix.
This is where symptoms need context.

NICE says hydrogen breath testing is not necessary to confirm IBS in people who already meet IBS diagnostic criteria 17. That is a good reminder that not every reader needs every test. At the same time, breath testing can be reasonable when the pattern raises a more specific SIBO or lactose question.
Use this table as the practical next-step filter:
| Situation | Better Next Step |
|---|---|
| Broad, chronic pain plus bowel habit change with no red flags | discuss IBS evaluation and management |
| Bloating and gas pattern plus overgrowth context | discuss SIBO breath testing in clinical context |
| Clear dairy, fructose, or sugar-alcohol reactions | use structured food testing or targeted intolerance review |
| Blood in stool, weight loss, fever, anemia, or later-life new symptoms | move medical evaluation higher than diet experiments |
If that last row is the real question now, stop using this page as the main sorting tool and switch to IBS vs colorectal warning signs.
What to track before that conversation:
| Track This | Why It Helps |
|---|---|
| specific food or food group | separates narrow intolerance from broader IBS patterns |
| amount eaten | shows whether dose matters |
| time to symptoms | helps distinguish immediate food reactions from broader all-day symptom patterns |
| bowel pattern across the week | shows whether symptoms are chronic and syndrome-like |
| surgery, diabetes, opioid use, or motility issues | adds context for SIBO plausibility |
And if the line still feels blurry, use this quick decision tree:
If you want the short version:
That last point matters most.
You do not need a better guess nearly as much as you need a better pattern. Track what repeats. Notice whether one food keeps showing up or whether the whole week is messy. Bring that pattern to your next conversation.
If symptoms are still confusing after you compare the three buckets, move to what to test next or use structured reintroduction and personalization to stop guessing from random single reactions.
If the confusion started during Step 2, read when every FODMAP challenge seems to fail for a cleaner decision tree.
Xam Riche is a gut health solopreneur and founder of YourFitNature, dedicated to helping people navigate digestive wellness through evidence-based information and personal experience. After years of struggling with IBS and bloating, Xam discovered the transformative power of the low FODMAP diet and now shares practical, science-backed guidance to help others find relief. While not a medical professional, Xam combines extensive research with lived experience to create accessible, empowering resources for the gut health community. Learn more about our mission
As an affiliate, we may earn from qualifying purchases.
Showing 10 of 140