
By Xam Riche on March 18, 2026 • 15 min read
This article is for informational and educational purposes only and does not constitute medical advice. Always consult with a registered dietitian, gastroenterologist, or other qualified medical professional before making significant dietary changes.
Finished elimination and not sure what comes next? This guide shows you how to reintroduce FODMAPs one group at a time, track symptoms clearly, and build a personalized diet without the chaos.
Short answer: reintroduction is the phase where you test one FODMAP group and one food at a time so you can turn elimination into a more personal, less-restrictive long-term diet.
This page is for you if elimination gave you a calmer baseline and your next question is: "How do I test foods without ruining the signal?"
Use a different page first if your elimination phase never really settled in When Low FODMAP Does Not Work: Next Steps, or if you need the bigger protocol overview in Low FODMAP Diet for Bloating: How It Helps & The 3 Phases Explained.

If reintroducing foods feels more stressful than elimination did, that makes sense.
This is the phase where many people worry about losing all the progress they fought for. One wrong meal can feel like it will send you straight back to bloating, pain, and bathroom urgency.
If urgency is making you afraid to liberalize the diet, read this guide to IBS-D and low FODMAP before you cut more foods.
You are not doing this wrong. You are just at the point where structure matters more than willpower.
Here is the truth: the reintroduction phase is not the risky part of the low FODMAP diet. Random testing is.
The goal of low FODMAP reintroduction is not to prove that your gut is "good" or "bad." The goal is to create a clean signal. You test one thing at a time, observe what happens, and use that data to build a diet you can actually live with.
If you still need the big-picture version first, start with our 3-phase Low FODMAP protocol. This guide is the step-by-step deep dive into Phase 2.
We are going to focus on the practical details that usually get rushed: timing, test foods, washouts, and what to do when a challenge goes sideways.
Start here. If your baseline is unstable, wait.
Monash advises that if you have followed the low FODMAP diet for 2-6 weeks and your IBS symptoms improved, it is time to move to Step 2 reintroduction, but only once symptoms are well controlled 1.
That means you are looking for a week where your symptoms are quieter and your routine is fairly predictable. You do not need perfection. You do need enough stability to notice whether the test food is the thing changing the picture.
You are probably ready if:
You are probably not ready yet if:
If that last point sounds familiar, stop and read Low FODMAP not working before pushing into reintroduction. If the baseline never improved, the next step may be troubleshooting, not testing.
Bottom line: do not start reintroduction because you are tired of elimination. Start because your baseline is stable enough to give you useful information.
This phase exists to personalize, not to restrict.
Clinical guidance describes the low FODMAP diet as a three-stage process in which reintroduction identifies triggers and personalization creates a less restrictive long-term diet with more variety 2.
That matters because many people accidentally turn Phase 1 into a forever diet. They keep avoiding foods, keep shrinking variety, and never get the clarity they were supposed to get from the protocol.
Here is the shift:
That is why words like "pass" and "fail" can be misleading. A reaction is not proof that your body is broken. It is data. It may tell you that:
Monash notes that foods containing the same FODMAP are not always interchangeable because different foods can contain very different amounts, and newer testing shows that food composition can change over time 3 4.
So no, one reaction does not automatically mean "I can never eat this whole category again."
The good news is that long-term personalized low FODMAP eating can improve symptoms while maintaining Bifidobacteria abundance, suggesting that reintroduction and personalization may normalize some effects of short-term restriction 5.
That broader microbiome-diversity angle matters beyond IBS mechanics too, which is part of why we now frame personalization as more than symptom control alone in our explainers on the gut-heart axis, the gut-liver axis, and the gut-kidney axis.
Bottom line: the point of reintroduction is food freedom with clearer boundaries, not permanent fear.
Once you have enough challenge data to personalize, use diet diversity after low FODMAP to rebuild variety without turning the next phase into random testing.
Most confusing reintroductions are not caused by the challenge food alone. They are caused by noise.
Noise looks like this:
Monash recommends using one challenge food at a time, recording symptoms in the app diary, and stopping early if unpleasant symptoms appear after the first or second day 6.
That is why your setup matters so much. Keep the rest of the week boring on purpose. Use familiar meals. Keep portions steady. If you need help holding that baseline, use a simple Low FODMAP meal plan and review how to avoid accidental stacking.
Your basic setup checklist:
If you want a digital tool instead of a paper diary, use the tracker below:
Monash states that during Step 2, the low FODMAP diet continues as your background diet while you challenge each FODMAP group separately over 3 days 7.
Monash also recommends completing each challenge over a 3-day period, then taking a 2-3 day break between challenges, or waiting until symptoms settle before the next challenge 8.
The structure is simple:
Here is the schedule in plain language:
| Day | Portion Goal | What to Track |
|---|---|---|
| 1 | Small | Bloating, pain, urgency, stool change |
| 2 | Medium | Symptom intensity, timing, cumulative effect |
| 3 | Larger challenge | Threshold response, delayed symptoms |
| 4-6 | Washout / reset | Return to baseline before the next challenge |

Keep the rest of the day low FODMAP. That is what turns the challenge food into useful data instead of just another random symptom day.
For example, if you are testing lactose, choose one lactose-containing food and increase the serve over 3 days while leaving everything else steady. You are not "seeing what happens if I eat normally again." You are running a controlled test.
Download the printable Reintroduction Tracker Worksheet to plan one challenge at a time and record what actually happened.
Bottom line: this is not about bravery. It is about reducing variables until the result makes sense.
According to Monash, there is no single "correct" order for FODMAP reintroduction. Many people start with a food they miss most, feel most confident about, or eat regularly 9.
That means you do not need to obsess over some perfect universal sequence. You do need a strategy.
Start with foods that are:
Monash gives examples like using wheat pasta to test fructans in grains, mango for excess fructose, and honey for higher-fructose challenge doses 10 11.
So if yogurt is the food you miss most, lactose may be a good place to start. If wheat is a staple in your life, fructans may deserve early clarity. If fruit tends to scare you, save fructose for a week when the rest of your routine is extra calm.
At a high level, the main groups you will work through are:
If you are unsure what to keep on your plate while you test, fall back on your safe baseline foods and keep the week simple.
Bottom line: choose a test food you can measure clearly and a FODMAP group you feel ready to face. Clarity beats bravery here too.
Not every symptom spike means the test "failed."
This is where a lot of people panic. They feel slightly off on day 2 and assume the entire category is out forever. But your job is to look for a pattern, not one isolated sensation.
Use a simple three-bucket interpretation model:
| Result | What It Usually Means | Next Move |
|---|---|---|
| Pass | Little to no symptom change across doses | Add the food back in normal rotation |
| Partial tolerance | Fine at lower dose, symptoms at higher dose | Keep the food at a smaller serve |
| Reactive | Clear symptoms early or repeatedly | Pause, reset, and retest later if needed |
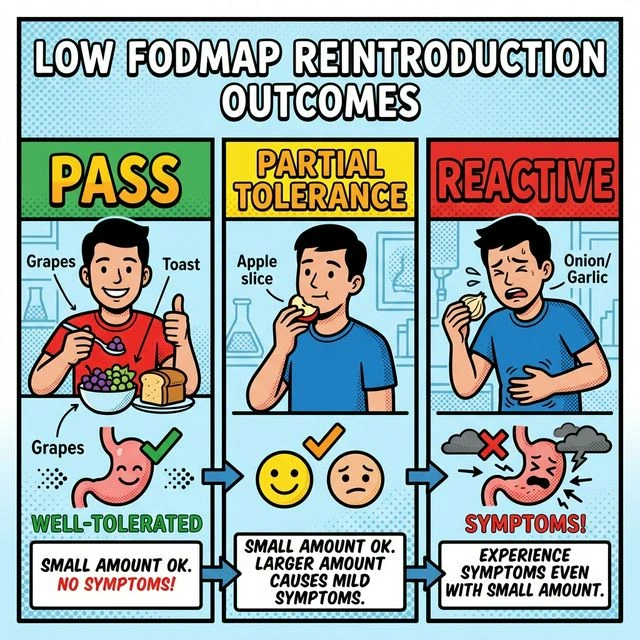
What should you actually track?
Monash also recommends tracking symptoms in the diary and stopping a challenge early if symptoms become unpleasant 12.
Here is the key idea: tolerance is often about dose and context, not just the food name. That is why one food in a FODMAP category may feel worse than another, and why one large serve may trigger symptoms even if a small serve does not.
Bottom line: if a reaction appears, ask "what did this teach me?" before you ask "what did I do wrong?"
First, stop. Then simplify.
If symptoms return during reintroduction, do this in order:
That last part matters. Sometimes the result is real. Sometimes the week was messy.
If your symptoms are confusing, ask:
This is where non-food factors matter. If your nervous system is already on edge, stress can distort symptoms and make food reactions feel louder than they are.
And if everything seems to trigger symptoms, or nothing improved even before reintroduction, step back and read what to do when Low FODMAP is not working. That is not failure. That is useful course correction.
If you want a fuller decision framework for what to do after a bad challenge, read when reintroduction fails.
If you cannot tell whether a reaction suggests a food trigger, a broader IBS flare, or something more like SIBO, start with this comparison guide.
This is the payoff.
Once you have a few tests behind you, stop thinking in terms of allowed and forbidden foods. Start building your personal FODMAP map.
| Bucket | What Goes Here | Reader Action |
|---|---|---|
| Safe | No meaningful symptoms | Eat normally |
| Limited | Tolerated only at smaller portions | Use strategically |
| Retest Later | Ambiguous or mixed result | Retry in a calmer week |
| Avoid for Now | Strong reaction | Pause and revisit later if needed |
In the 2024 blinded reintroduction trial, IBS responders had an average of 2.5 FODMAP triggers each, and the most common triggers were fructans and mannitol, followed by GOS, lactose, fructose, and sorbitol 13.
That tells us something important: your trigger profile is likely to be mixed and personal. You are not trying to discover one villain. You are trying to discover your own pattern.
Over time, this moves you into the personalization phase. That is where the diet becomes sustainable. That is where variety comes back. That is where you stop living inside Phase 1. If Step 3 feels compliant on paper but still chaotic in real life, use low-FODMAP personalization mistakes for the execution-error reset path before you shrink the diet again.
NICE recommends that exclusion diets such as the low FODMAP diet should only be delivered by a healthcare professional with expertise in dietary management 14. If your results feel messy, restrictive, or emotionally exhausting, that is a good reason to bring in a GI-focused dietitian.
Bottom line: the goal is not to win elimination. The goal is to build the widest, calmest, most functional diet your body can handle.
If you want the shortest version of this whole article, here it is:
Start with one challenge food this week.
Block out a calmer stretch of days. Keep your background meals simple. Use the interactive tracker or worksheet. Then review what the test actually taught you before moving on.
If the holiday calendar is getting chaotic, read this low-FODMAP holiday survival guide before you decide whether to pause the challenge or simplify the rest of the week.
If your reintroductions keep going badly, do not keep forcing it. Revisit the full 3-phase guide, tighten the baseline with the meal plan, or move into troubleshooting.
The good news is that this phase is where the diet stops feeling like restriction and starts becoming useful.
Xam Riche is a gut health solopreneur and founder of YourFitNature, dedicated to helping people navigate digestive wellness through evidence-based information and personal experience. After years of struggling with IBS and bloating, Xam discovered the transformative power of the low FODMAP diet and now shares practical, science-backed guidance to help others find relief. While not a medical professional, Xam combines extensive research with lived experience to create accessible, empowering resources for the gut health community. Learn more about our mission
As an affiliate, we may earn from qualifying purchases.
Showing 10 of 127