
By Xam Riche on April 24, 2026 • 14 min read
This article is for informational and educational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional before using symptom information to make diagnosis or treatment decisions.

IBS can turn the body into a constant alarm system. Pain, bloating, urgency, or constipation create fear. Fear raises vigilance. Vigilance makes the gut feel louder. If anxiety or low mood are now part of the story, the answer is not to pretend the symptoms are imaginary. The answer is to widen the treatment frame.
Short answer: anxiety and depression commonly overlap with IBS, and that overlap can make symptoms feel more intrusive, more threatening, and harder to settle. That does not mean IBS is "all in your head." It means the brain-gut loop may need direct treatment instead of asking diet alone to do the entire job.
This page is for you if IBS symptoms and mental health strain are starting to reinforce each other, and you need a clearer next step than another round of food restriction.
Use a different page first if you still are not sure the pattern is IBS at all, or if food-trigger sorting is clearly the bigger issue. Start with when low FODMAP does not work, SIBO vs IBS vs food intolerance, or the practical gut-brain pillar at stress-bloating-through-gut-brain-axis.
Use this selector when the gut-brain shelf starts to feel too abstract.
| If the loudest issue is... | Best next read | Why |
|---|---|---|
| Fear, anticipation, low mood, or the symptom loop is taking over daily life | This page | It owns the mood-loop and care-lane conversation without saying symptoms are imaginary. |
| Urgency, diarrhea, fast transit, or serotonin-targeted IBS-D options | Serotonin and IBS-D | It keeps urgency-heavy patterns in the IBS-D mechanism and treatment lane. |
| How gut contents become serotonin, motility, urgency, and pain signals | Enterochromaffin cells, serotonin, and gut pain signaling | It explains the upstream cell-level bridge without turning it into a self-treatment plan. |
| Pain volume, stress sensitivity, sex or hormone context, or persistent visceral pain | Stress, sex, and chronic visceral pain | It routes pain amplification into the pain-threshold anchor. |
| The pattern is mixed, persistent, medication-adjacent, or hard to summarize | Doctor visit prep for IBS next steps | It turns mechanism reading into a cleaner clinician handoff. |
The older version of this topic drifted into a broad literature summary and a side conversation about eating-disorder screening. That is not the best role for this slug inside the current ecosystem.
This page works better as an IBS mental-health bridge:
The core reader question is simple:
What should I do when IBS symptoms and mood burden are feeding each other?
IBS is not just a bowel-speed problem. MedlinePlus says the intestine is connected to the brain by hormone and nerve signals that go back and forth between the bowel and the brain, and stress can make the intestines more sensitive and contract more 1.
NCCIH goes even further and describes IBS as a disorder of how the brain and gut work together 2.
That helps explain why anxiety and depression come up so often in IBS care. They are not random side notes. They can change:
The safest way to say it is this:
anxiety and depression often overlap with IBS, can worsen the illness burden, and may need treatment as part of the IBS plan, but they do not erase the gut side of the condition.
A 2017 systematic review and meta-analysis found that anxiety and depression symptom levels were significantly higher in IBS patients than in healthy controls across IBS subtypes 3.
A separate meta-analysis found that baseline anxiety and depression were each associated with about a twofold higher risk of later IBS onset in the included studies 4.
Those findings matter, but they do not prove one clean one-way story where mood simply causes IBS. The better interpretation is that the relationship is bidirectional and layered:
That is exactly why narrow one-lever plans fail so often.
This overlap rarely shows up as a tidy textbook problem. More often, it looks like one of these patterns.
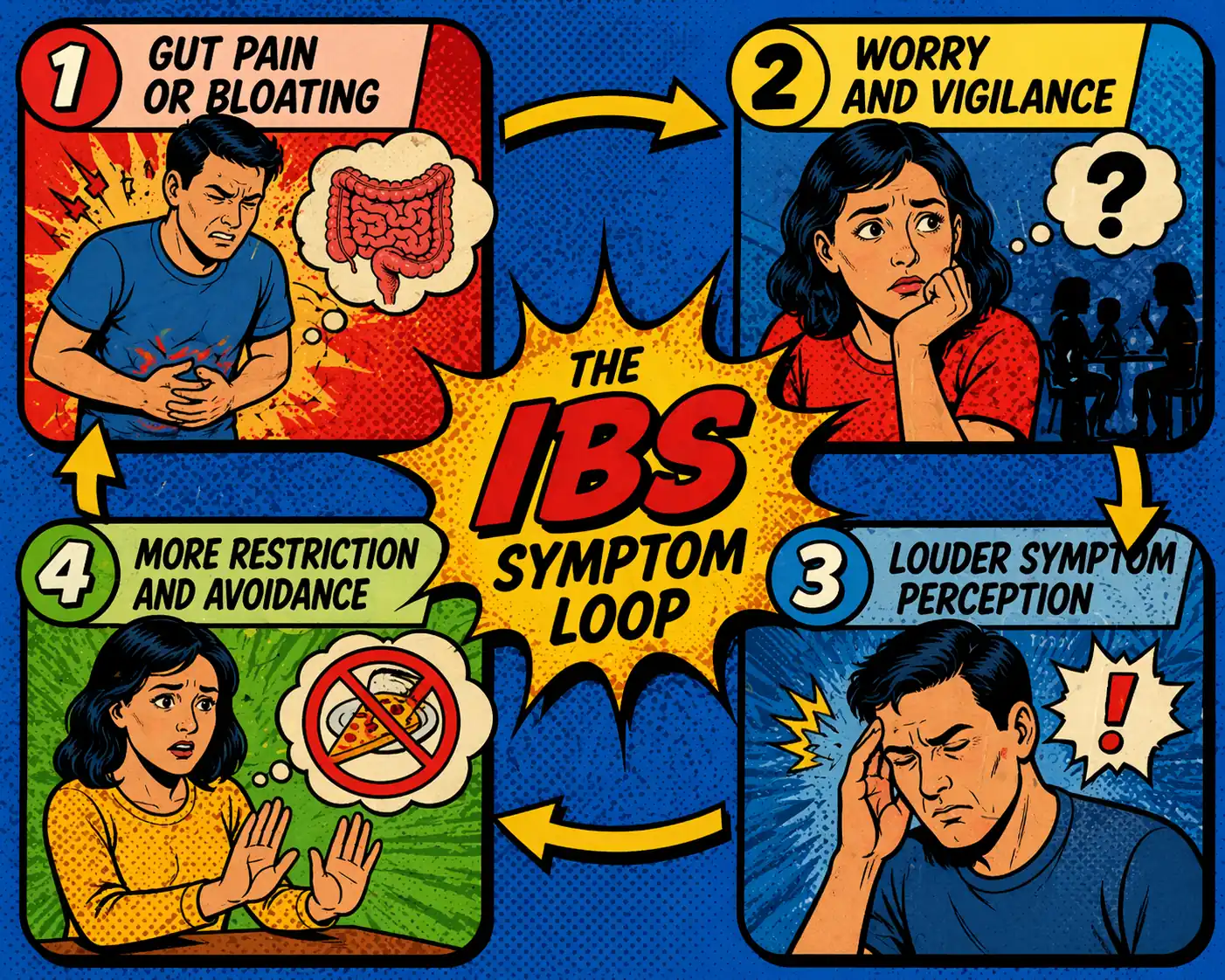
You eat the same meal you tolerated last week. This week it feels completely different.
That does not automatically mean the food changed. It can mean the nervous system changed. If that sounds familiar, the practical parent page is stress-bloating-through-gut-brain-axis.
You start feeling worse before the commute, before the meeting, before the restaurant meal, or before leaving the house.
That kind of anticipatory amplification fits the deeper science page at stress-irritable-bowel-syndrome-ibs.
When symptoms stay unpredictable, many people keep narrowing the menu. The diet becomes stricter, but the relief does not scale with the effort.
That usually means you need a broader troubleshooting frame, not a harsher food rulebook. Use when low FODMAP does not work when you are not sure whether the problem is hidden triggers, a missed diagnosis, or a loud gut-brain loop.
You cancel plans. You brace before meals. You check your abdomen all day. You do not trust your body.
At that point, the burden is no longer just digestive. It is also behavioral, emotional, and quality-of-life related. That is usually the moment when the plan needs to widen beyond self-guided diet work.
NIDDK says doctors may treat IBS with food changes, lifestyle changes, medicines, probiotics, and mental health therapies 5.
That treatment list only makes sense if IBS is a real disorder with multiple levers. Mental health support appears in IBS care because the brain-gut loop is part of the disease burden, not because doctors think the symptoms are fake.
So if you have been hearing "it is probably stress" as a dismissal, replace it with a more accurate sentence:
stress, anxiety, and depression can change the way real IBS symptoms are processed, amplified, and managed.
Diet work is useful when the main problem is a food pattern: a high-FODMAP trial that was never clean, a clear caffeine or alcohol trigger, a large fiber jump, or a meal-timing pattern that keeps flares predictable.
It becomes the wrong lead tool when every symptom sends you back into more restriction while the actual burden keeps spreading:
That is the moment to widen the plan. You may still need food troubleshooting, but food should not be asked to do the work of pain care, nervous-system care, therapy, medication review, or diagnostic follow-up.
If the diet trial itself still feels messy, use when low FODMAP does not work. If the pattern now looks more like a gut-brain pain-volume problem, the next layer is visceral hypersensitivity in IBS.
IBS overlap is rarely one clean lane. A person can have real bowel changes, real pain sensitivity, and real anxiety or depression at the same time.
One common loop looks like this:
| What changes | How it can reinforce the loop |
|---|---|
| Anxiety or anticipation rises | The body scans harder for gut sensations before meals, travel, work, or social plans. |
| Pain sensitivity is high | Normal digestion, gas, or stool movement can feel more intense than expected. |
| Urgency appears | Bathroom fear makes the next outing feel risky, even before eating. |
| Low mood sets in | Energy for planning, cooking, movement, therapy, or appointments drops. |
This is still not a self-diagnosis map. It is a routing map.
For pain that feels louder than the visible gut explanation, use visceral hypersensitivity in IBS or the deeper chronic pain page at stress, sex, and chronic visceral pain. For urgency-heavy IBS-D, read serotonin and IBS-D. For the cellular signaling layer behind serotonin-related pain and motility questions, go to enterochromaffin cells, serotonin, and gut pain signaling. If the main pattern is a fast bathroom run after eating, start with urgency after meals before assuming the whole problem is mood.
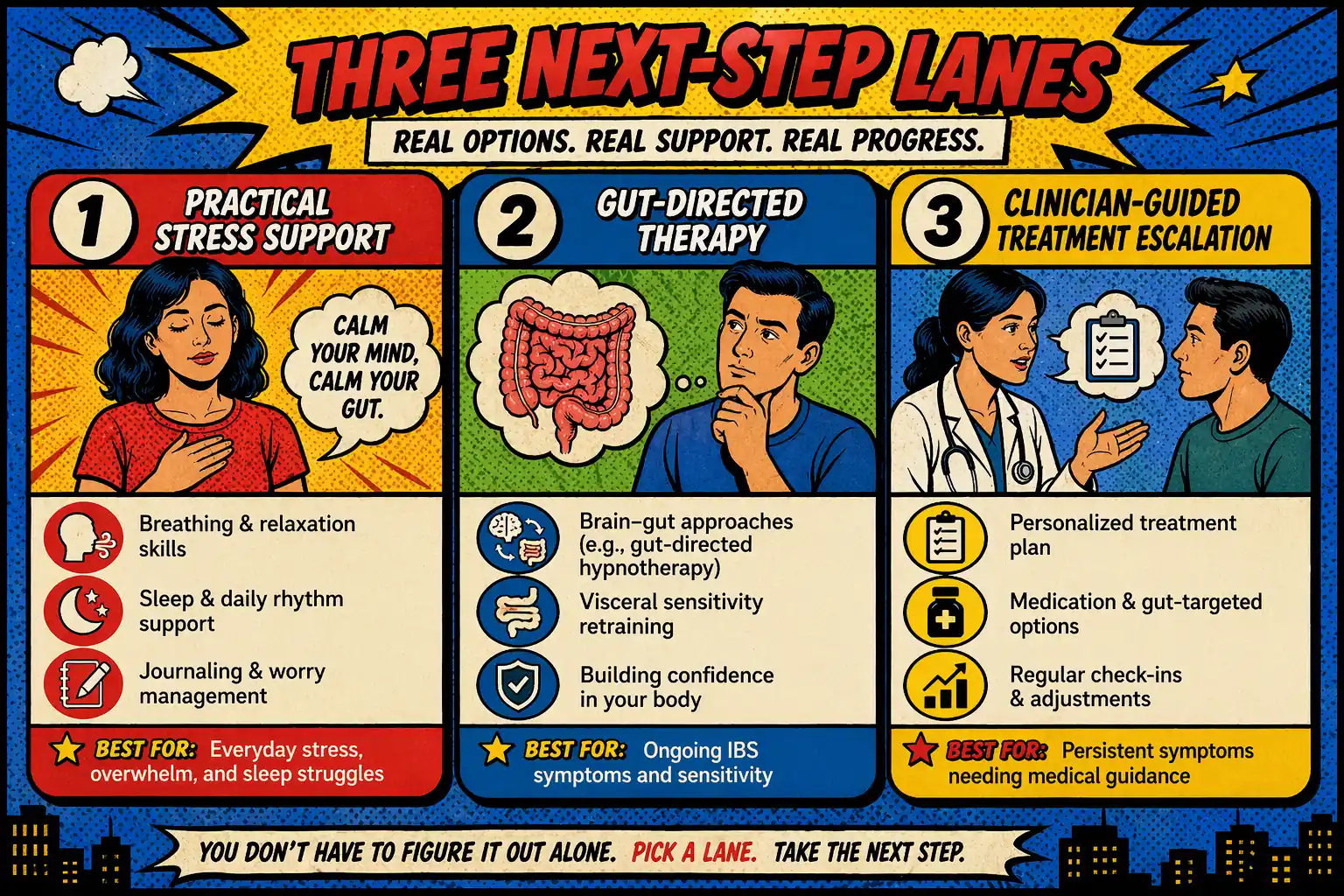
The next step depends on what is dominant now.
Start with the practical nervous-system page: stress-bloating-through-gut-brain-axis.
NIDDK says doctors may recommend cognitive behavioral therapy, gut-directed hypnotherapy, or relaxation training for IBS 6.
NCCIH says there is some evidence that gut-directed hypnotherapy can help IBS symptoms and improve health-related quality of life, and it notes that hypnotherapy and other psychological therapies can perform similarly in some analyses 7.
If that is the decision you are trying to make, go to gut-directed-hypnotherapy-for-ibs.
NIDDK also notes that low-dose antidepressants may be used for abdominal pain in IBS 8.
That route fits ibs-treatment when you need a clinician-guided escalation map.
Do not overfit everything to mental health if the basic gut picture is still unclear.
If upper-abdominal fullness, nausea, or early satiety dominate, go to functional dyspepsia. If the main confusion is whether this is really IBS, SIBO, or food intolerance, use SIBO vs IBS vs food intolerance.
Use this section when you are stuck between gut care and mental health care and do not want the appointment to collapse into "it is probably stress" or "just cut out more foods."
Bring a short pattern summary instead of a long diary:
| Bring this | Why it matters |
|---|---|
| Top 2 gut symptoms | Clarifies whether pain, urgency, constipation, diarrhea, bloating, or nausea is leading. |
| Mood and stress pattern | Shows whether anxiety, low mood, panic, sleep loss, or anticipation are part of the flare cycle. |
| Food work already tried | Prevents endless diet resets when the trial was already reasonable. |
| Current medicines and supplements | Helps a clinician check interactions, side effects, constipation risk, diarrhea risk, and pain options. |
| Safety changes | Keeps bleeding, weight loss, fever, severe new pain, vomiting, or rapidly changing symptoms out of self-management. |
Useful questions to ask:
Download: IBS Mood Symptom Loop Conversation Guide
Once diet is no longer the whole explanation, the next step should match the dominant pattern rather than the scariest theory.
| If this is loudest now | Better next lane |
|---|---|
| Pain feels amplified or disproportionate | Read stress, sex, and chronic visceral pain. |
| Urgency is the main quality-of-life problem | Compare serotonin and IBS-D with urgency after meals. |
| Bathroom fear, access planning, or avoidance is the specific loop | Use the bathroom anxiety route map for IBS. |
| Hunger, fullness, cravings, and gut signals feel blended together | Use gut-brain signaling and appetite. |
| Anxiety, low mood, or panic feels persistent | Bring the conversation guide to a clinician or therapist instead of trying to solve it through food rules alone. |
Two different escalation paths matter here.
If you have alarm features, rapidly changing symptoms, bleeding, unexplained weight loss, persistent vomiting, or a diagnosis that no longer feels stable, step out of gut-brain self-sorting and get evaluated.
NIMH advises seeking professional help when severe symptoms have lasted 2 weeks or more and getting immediate help for thoughts of suicide or urges to hurt yourself 9.
If you are in the United States, NIMH directs people in suicidal crisis or emotional distress to call or text 988 for immediate help 10.
IBS, anxiety, and depression often travel together because the gut and brain keep talking to each other. That overlap can make symptoms feel louder, more frightening, and harder to stabilize. It still does not mean the illness is imaginary.
What it means in practice is simpler: if the symptom loop now includes fear, anticipation, low mood, or exhausting self-monitoring, the next move may need to include therapy, broader treatment, or direct mental health support instead of another attempt to fix everything through food alone.
If migraine also travels with the IBS pattern, use the migraine and IBS overlap bridge to separate gut-brain comorbidity from migraine-specific care.
For a practical therapy-skills bridge, CBT for IBS anxiety, urgency, and gut-brain skills separates gut symptoms from the fear, avoidance, and urgency loops that can grow around them.
Xam Riche is a gut health solopreneur and founder of YourFitNature, dedicated to helping people navigate digestive wellness through evidence-based information and personal experience. After years of struggling with IBS and bloating, Xam discovered the transformative power of the low FODMAP diet and now shares practical, science-backed guidance to help others find relief. While not a medical professional, Xam combines extensive research with lived experience to create accessible, empowering resources for the gut health community. Learn more about our mission
As an affiliate, we may earn from qualifying purchases.
Showing 10 of 152