
By Xam Riche on May 8, 2026 • 6 min read
This article is for informational and educational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional before using symptom information to make diagnosis or treatment decisions.
Sometimes the food looks safe and the meal still backfires.
You checked the app. You picked the low-FODMAP option. You chose a protein bar with a clean-looking label, avocado in a measured portion, sugar-free gum, or a restaurant meal that avoided garlic and onion. Then reflux, fullness, bloating, or urgency showed up anyway.
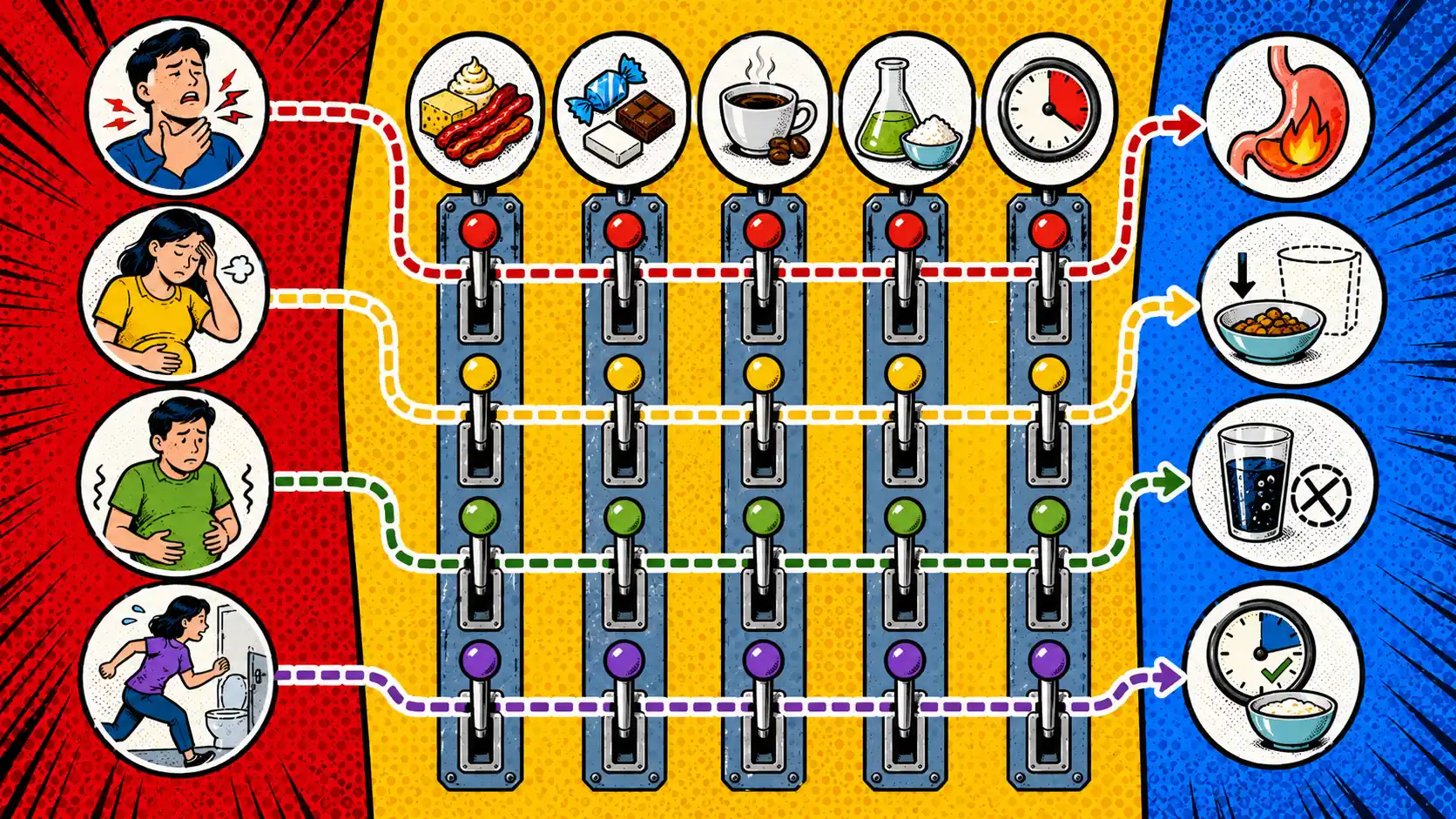
That does not always mean the food is secretly forbidden. It may mean the meal format was louder than the ingredient list. Fat load, sugar alcohols, added fibers, caffeine, carbonation, meal size, and timing can all change the symptom pattern.
Use this page when the food list is not enough. If product ingredients are the main issue, keep hidden FODMAPs in products open. If urgency dominates, use IBS-D and low FODMAP. If the main question is the urgent bathroom run after eating, use urgency after meals. If burning or early fullness dominates, route to reflux-like symptoms or functional dyspepsia.

Low-FODMAP lists answer one question: does this serving contain a concerning FODMAP load? They do not answer every post-meal symptom question.
A meal can still be noisy because it is:
That is why the next test should often be a simpler meal format, not a stricter food list.
Fat is not bad. Avocado, nuts, oils, seeds, fish, eggs, and plant-based fats can fit many diets. But a high-fat or rich meal can be a symptom-context lever for some readers.
If burning, sour taste, regurgitation, or chest-throat discomfort dominates, use reflux-like symptoms. NIDDK notes that clinicians may recommend avoiding foods and drinks that worsen GERD symptoms, eating earlier before lying down, and changing meal habits 1.
If early fullness, nausea, upper-stomach heaviness, or post-meal discomfort is the main pattern, use functional dyspepsia. If urgent loose stools are the loudest issue, use IBS-D and low FODMAP.
Persistent watery diarrhea that is worse after fatty meals deserves a wider clinical lens. Research has found bile acid malabsorption in a subset of patients with IBS-D-type symptoms 2. That does not mean every post-fatty-meal reaction is bile-acid related. It means persistent watery diarrhea should not be handled by endless food cutting alone.
Sugar-free does not mean symptom-free.
Polyols are sugar alcohols such as sorbitol, mannitol, xylitol, maltitol, and isomalt. They can appear in gums, mints, candies, protein bars, powders, drinks, and "no sugar" products. Monash identifies polyols as particularly relevant for IBS and discusses sorbitol and mannitol symptom effects in IBS research 3.
Monash's label-reading guidance also warns readers to be careful with low-sugar or no-sugar products when polyol tolerance is an issue and notes that added prebiotic fibers can cause gas, bloating, or distension in some people with IBS 4.
So if symptoms show up after gum, mints, sugar-free drinks, protein bars, or "gut-friendly" snacks, the question may be the label, not your willpower.
Front labels are often too vague for IBS troubleshooting. The useful clues are in the ingredient list:
If the product is a protein item, use the low-FODMAP vegetarian protein guide before assuming powders are easier than food anchors. If the broader product pattern is confusing, use hidden FODMAPs in products.
Download: Post-Meal Trigger Audit and Product Label Trigger Checklist
Use a seven-day audit:
For beverages, use coffee, tea, and gut symptoms. For restaurant patterns, use low-FODMAP eating out. For plant-pattern questions, use plant-based eating and gut symptoms. If the recurring issue is avocado, nuts, oils, seeds, or rich plant-forward meals, use avocado, nuts, and plant fats for a more focused plant-fat test.
| If this is the main pattern | Best next read |
|---|---|
| Product labels are confusing | Hidden FODMAPs in products |
| Urgency dominates | Urgency after meals |
| Burning or regurgitation dominates | Reflux-like symptoms |
| Early fullness or nausea dominates | Functional dyspepsia |
| Coffee or tea is involved | Coffee, tea, and gut symptoms |
| Beer, wine, cocktails, or mixers are involved | Beer, wine, cocktails, and gut symptoms |
| Skipped meals, grazing, or late meals dominate | Meal timing and gut symptoms |
| The issue is restaurants | Low-FODMAP eating out |
| Avocado, nuts, oils, or seeds dominate | Avocado, nuts, and plant fats |
A food list is useful, but it is not the whole meal.
Before you ban another ingredient, test the format. Was the meal rich? Was the product sweetened with polyols? Was there added fiber? Was caffeine involved? Was the symptom reflux, fullness, bloating, or urgency?
The better question is not "Is this food good or bad?" It is "Which lever made this meal louder?"
Xam Riche is a gut health solopreneur and founder of YourFitNature, dedicated to helping people navigate digestive wellness through evidence-based information and personal experience. After years of struggling with IBS and bloating, Xam discovered the transformative power of the low FODMAP diet and now shares practical, science-backed guidance to help others find relief. While not a medical professional, Xam combines extensive research with lived experience to create accessible, empowering resources for the gut health community. Learn more about our mission
As an affiliate, we may earn from qualifying purchases.
Showing 10 of 143