
By Xam Riche on April 24, 2026 • 10 min read
This article is for informational and educational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional before using symptom information to make diagnosis or treatment decisions.

A burning chest, sour taste, or throat irritation can sound simple on paper and still be messy in real life. Some upper-GI flares fit reflux cleanly. Others start looking more like indigestion, functional dyspepsia, medicine-related irritation, or a pattern that needs medical review instead of more guesswork.
Short answer: reflux-like symptoms often include heartburn, regurgitation or sour taste, and symptom flares after meals, lying down, or bending over. But those symptoms do not automatically prove GERD, and they should be sorted against nearby upper-GI patterns before you lock yourself into one label.
This page is for you if your confusion starts with burning in the chest, sour taste, throat irritation, or upper-GI discomfort that seems worse after eating or when you lie down.
Use a different page first if the louder clue is early fullness, meal heaviness, nausea after a few bites, or the sense that food just sits there. That pattern fits functional dyspepsia better. If the bigger problem is broader IBS-style troubleshooting after diet changes, go to when low FODMAP does not work.
This page is deliberately not calling every upper-GI burning episode "GERD."
NIDDK distinguishes gastroesophageal reflux (GER) from GERD. GER is the backflow of stomach contents into the esophagus. GERD is the more persistent or complicated version, where reflux causes repeated symptoms or leads to problems over time 1.
That distinction matters because many readers do not arrive with a confirmed diagnosis. They arrive with:
Doctors often diagnose GER or GERD from symptoms and history first, then widen to testing if symptoms suggest complications, another cause, or poor response to treatment 2.
So the right first question is usually not "Do I definitely have GERD?" It is:
Does this look like a reflux-dominant pattern, a different upper-GI pattern, or a situation that should stop being self-sorted?
NHS lists the main symptoms of acid reflux as:
It also notes that some people have:
and that symptoms are often worse after eating, when lying down, and when bending over 3.
That does not mean every cough, throat symptom, or chest discomfort is reflux. It means those clues belong in the pattern review when they repeatedly cluster with classic reflux features.
Use the symptom pattern, not the label, to decide what to do next.
Official patient guidance is fairly consistent on the common aggravators.
NHS and MedlinePlus both describe reflux symptoms as being made worse by common factors such as trigger foods, overweight or obesity, smoking, pregnancy, and lying down too soon after eating 4 5.
NHS also includes stress, anxiety, some medicines such as anti-inflammatory painkillers, and hiatus hernia in its indigestion guidance 6.
That means a reflux-leaning pattern often becomes more plausible when:
The point is not to memorize a trigger list. The point is to notice when the pattern behaves like reflux often enough that it deserves a cleaner next step.

This is the most important nearby distinction in the current content ecosystem.
NIDDK's indigestion guidance says doctors may diagnose functional dyspepsia when upper-abdominal pain, burning, discomfort, or feeling full too soon while eating fits the picture and another cause is not found 7.
That means reflux-like symptoms and dyspepsia can overlap, but they are not the same question.
| Pattern | Common clues | Better next page |
|---|---|---|
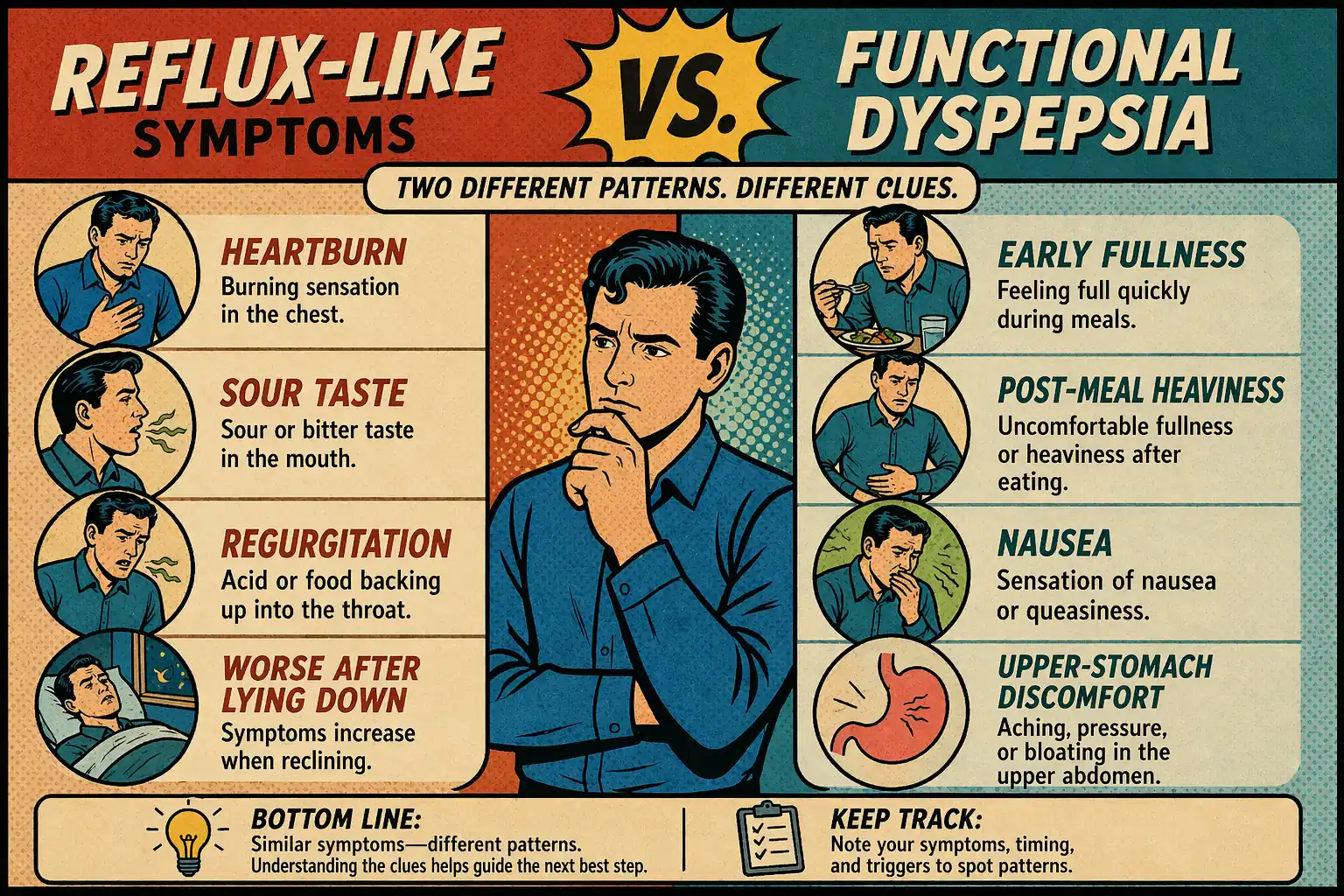
| Reflux-like symptoms | heartburn, sour taste, regurgitation, worse after lying down or bending | this page first |
| Functional dyspepsia pattern | early fullness, post-meal heaviness, nausea, upper-stomach discomfort, pain or burning without a simple reflux story | functional dyspepsia |
| Broader troubleshooting pattern | food changes are failing, symptoms are mixed, lower-GI overlap is strong, or another diagnosis may fit better | when low FODMAP does not work |
Use that table as a routing tool, not a diagnosis.
If the loudest sentence in your head is, "I get burning and sour taste when I lie down," reflux moves higher on the list.
If the loudest sentence is, "A few bites make me feel overfull, nauseated, or heavy in the upper stomach," then the functional dyspepsia frame usually earns more attention.
If the question is more about whether a small food-first option fits nausea or unsettled upper-GI discomfort, use the ginger guide as a fit check, especially because ginger can irritate reflux in some people.
If you are not even sure whether the real problem is food-trigger bloating, lower-GI IBS overlap, or upper-GI discomfort, step sideways first to why healthy foods still cause bloating.
For a mild, familiar reflux-like pattern, official self-care advice is fairly simple.
NHS recommends:
For readers testing whether coffee, tea, or caffeine is part of the pattern, coffee, tea, and gut symptoms keeps the reflux question separate from IBS urgency and microbiome claims.
When reflux seems tied to rich meals, sugar-free products, protein bars, or mixed post-meal symptoms, use fat, sugar alcohols, and post-meal symptoms to separate fat load, polyols, fullness, and urgency before blaming one food.
8.
NIDDK and MedlinePlus make similar points about weight loss when relevant, avoiding meals close to lying down, and avoiding repeated trigger foods 9 10.
That gives you a reasonable short list:
If you already tried the usual food-first moves and the picture is still messy, do not keep tightening the same loop. Move next to when low FODMAP does not work.
This is the boundary line that matters most.
NHS says to see a GP if lifestyle changes and pharmacy medicines are not helping, if you have heartburn most days, or if you have symptoms such as food getting stuck, frequent vomiting, or weight loss for no clear reason 11.
Its indigestion guidance adds other escalation clues such as severe pain, difficulty swallowing, repeated vomiting, iron deficiency anemia, a lump sensation, or bloody vomit or poo 12.
NIDDK also notes that doctors may order tests when symptoms suggest complications, suggest another condition causing similar symptoms, or do not improve after treatment and lifestyle changes 13.
So stop self-sorting and get medical review if you have:
And treat chest pain with shortness of breath, jaw pain, or arm pain as an urgent medical problem, not a reflux question 14.

Reflux-like symptoms are common, but the label gets sloppy fast.
The more useful sequence is:
This page should help you avoid two common mistakes:
Download: Reflux-Like Symptom Discussion Checklist
Use this split before cutting more foods:
| Pattern | Better route |
|---|---|
| Burning, sour taste, throat irritation, worse lying down | Stay with this reflux-like symptom guide. |
| Early fullness, nausea, or upper-abdominal heaviness | Functional dyspepsia and gut-brain communication. |
| Urgency, diarrhea, or lower-abdominal cramping after meals | Urgency after meals. |
| Symptoms follow beer, wine, cocktails, or late rich meals | Beer, wine, cocktails, and gut symptoms. |
| Symptoms appear during or after exercise | Movement, exercise, and gut symptoms. |
The food-trigger boundary is simple: reflux-like symptoms can respond to timing, meal size, alcohol, caffeine, and rich-meal changes, but swallowing trouble, bleeding, weight loss, persistent vomiting, severe pain, or chest pain with shortness of breath is not a diet experiment.
If reflux-like symptoms follow kombucha, kefir, sauerkraut, kimchi, wine, aged cheese, or vinegar-heavy foods, use histamine, fermented foods, and gut symptoms to separate acidity, carbonation, alcohol, dose, and histamine-style clues.
Reflux-like symptoms should be sorted by pattern before they become a generic food-trigger project. Burning, sour taste, upper-GI heaviness, urgency, alcohol, exercise, and red flags point to different next reads. Use the checklist to keep the story clear.
Xam Riche is a gut health solopreneur and founder of YourFitNature, dedicated to helping people navigate digestive wellness through evidence-based information and personal experience. After years of struggling with IBS and bloating, Xam discovered the transformative power of the low FODMAP diet and now shares practical, science-backed guidance to help others find relief. While not a medical professional, Xam combines extensive research with lived experience to create accessible, empowering resources for the gut health community. Learn more about our mission
As an affiliate, we may earn from qualifying purchases.
Showing 10 of 152