
By Xam Riche on April 28, 2026 • 13 min read
This article is for informational and educational purposes only and does not constitute medical advice. Always consult with a registered dietitian, gastroenterologist, or other qualified healthcare professional before making major diet changes, especially if IBS, constipation, severe bloating, or food intolerance symptoms are active.

You hear that gut microbes ferment fiber into useful compounds. Then you try to eat more beans, oats, resistant starch, or a prebiotic-heavy product and end up tight, noisy, and confused. At that point, the advice sounds self-contradictory. If fermentation is supposed to help the gut, why can it also make your abdomen feel worse by dinner?
Short answer: fiber fermentation is one of the main ways microbes turn undigested carbohydrates into relevant metabolites, including short-chain fatty acids or SCFAs. But the same process can also generate gas and symptom load. That is why fermentation belongs in both the microbiome-support story and the bloating story 1 2.
This page is for you if you already know fiber matters and now want to understand why fermentable fiber can feel useful in theory yet rough in practice.
Use a different page first if your main question is the category definition of prebiotic fiber, the broader interpretation of fiber diversity and microbiome resilience, or the downstream metabolite shelf on short-chain fatty acids. If your real problem is symptom sorting rather than mechanism, move sooner to why you still feel bloated after eating 'healthy' foods.
This article explains one narrower but important point:
Fermentation is not automatically the problem and not automatically the solution. It is the mechanism that helps explain both.
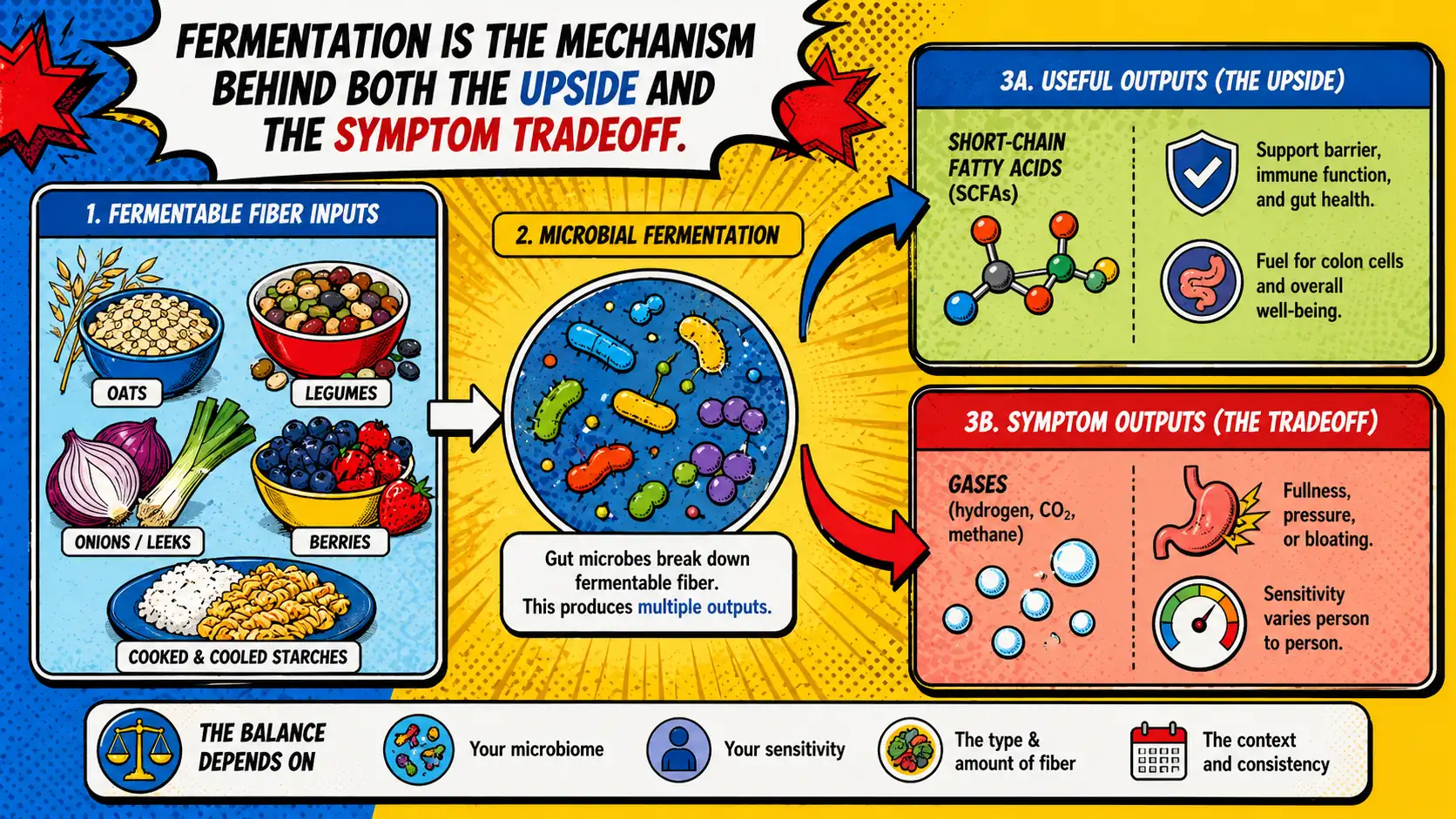
Fiber fermentation usually means gut microbes break down carbohydrates that your own small intestine did not fully digest. That matters because most dietary fibers are not one uniform substance. They differ in structure, fermentability, viscosity, and how much microbial access they create 3 4.
That is already more useful than the internet's usual framing.
The wellness version of the story says fiber feeds the good bacteria. The skeptical version says fiber just makes people gassy. Neither version is complete enough to guide a real decision.
Fermentation is simply a gut process. In the right context, it helps explain why fiber, prebiotics, and resistant starch keep appearing in microbiome science. In the wrong context, it also helps explain why the same foods can create more pressure, more fullness, and more second thoughts.
If your question is about fermented foods such as kimchi, sauerkraut, kefir, yogurt, miso, tempeh, or kombucha rather than fiber fermentation inside the colon, use fermented foods and gut health for the food-category and tolerance map.
This is also why the page sits below the broader prebiotic fiber bridge and beside fiber diversity and microbiome resilience. Those pages explain the category logic and the substrate-variety logic. This page explains why the experience of fermentation can still split into an upside and a downside.
Microbes ferment fiber because it gives them a usable substrate.
That fermentation can produce microbial metabolites such as acetate, propionate, and butyrate, which is one reason the SCFA story keeps showing up in gut-health education 5. If you want the deeper metabolite shelf after this section, move next to short-chain fatty acids.
But useful metabolites are not the only outputs.
Fermentation can also produce gases such as hydrogen, methane, and carbon dioxide, which means the same meal that is microbiome-relevant can also feel symptom-heavy 6 7.
That is where many readers get trapped. They imagine two clean possibilities:
Real guts are not that binary.
Gas does not automatically mean damage. But gas also does not automatically mean the current strategy fits your symptoms. The more useful question is:
What kind of fermentation burden did this food create, and could this gut handle it well?
One of the most useful updates in the IBS-and-fiber literature is that the old soluble-versus-insoluble split does not explain enough on its own 8.
What often matters more is functional behavior:
That is where rapidly fermented oligosaccharides enter the story. Monash's clinical summary explains that fibres fermented more quickly, including some FODMAP-linked oligosaccharides, may exacerbate symptoms via gas production, while slower-fermenting fibres such as psyllium are less likely to induce symptoms via gas accumulation 9.
That does not mean rapidly fermented fibres are fake or useless.
It means they can create a faster, louder symptom load in some guts.
This also helps explain why one person can tolerate oats or a cooled potato meal reasonably well, then react badly to a chicory-root blend, an inulin-heavy bar, or a meal stacked with onions, garlic, legumes, and a large serving size.
A food matrix matters too. A whole-food exposure and a concentrated prebiotic ingredient do not always land the same way in real life. If your main question is which food-source groups are gentler starting points, use food-first prebiotic fiber sources. If your question is whether wider substrate variety matters, use fiber diversity and microbiome resilience.
The practical point is simpler than the science:
Different fibers create different fermentation experiences.
That is one reason "just eat more fiber" can be terrible advice when symptom tolerance is the real bottleneck.
It would be convenient if the story ended with gas production.
It does not.
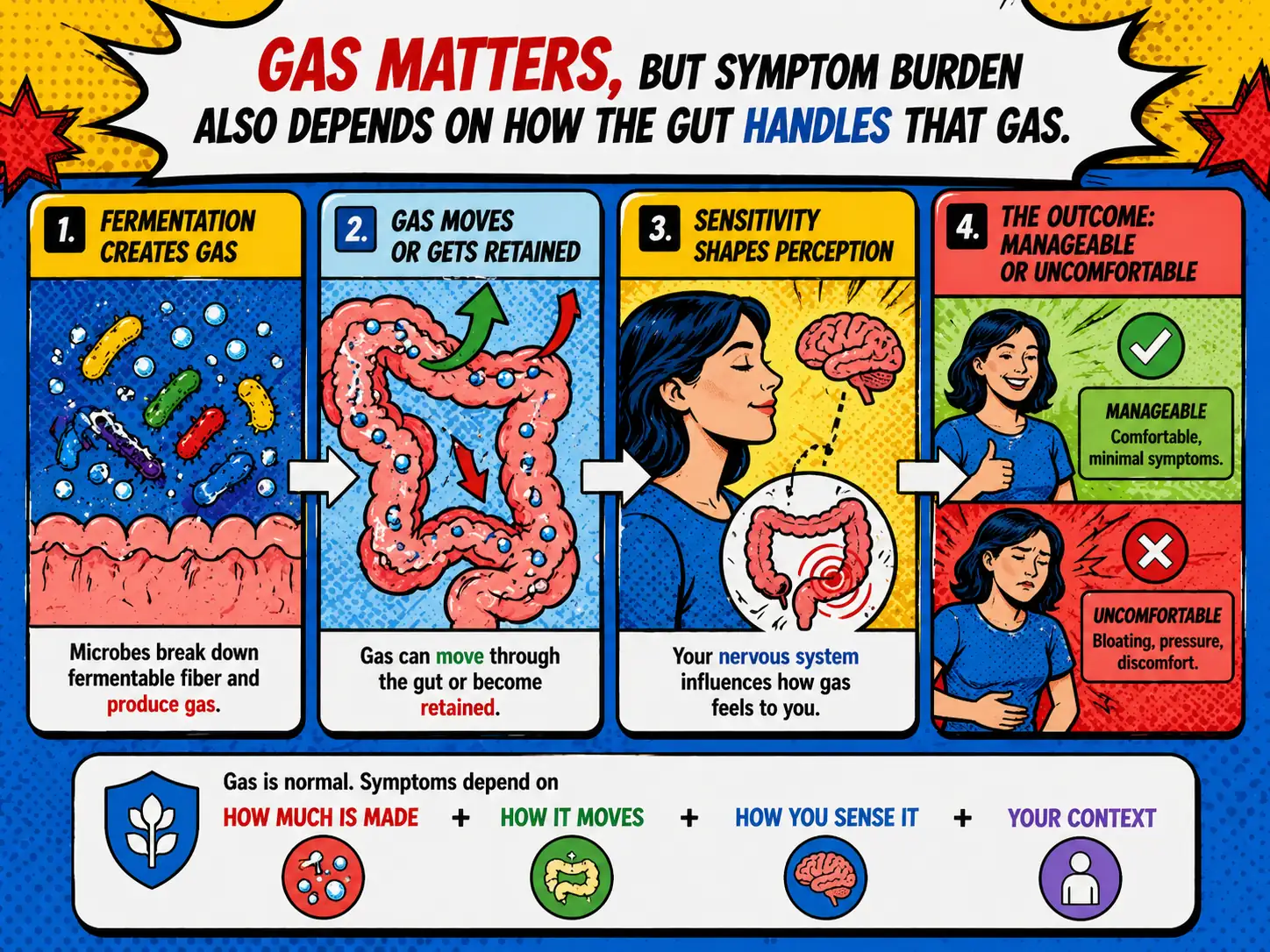
The OmniHeart trial notes that colonic bacteria produce gas by fermenting incompletely digested foods, including fibers, but also points out that fiber may impair gas transition and promote gas retention 10. A controlled study in healthy volunteers similarly found that a high-fibre diet promoted more gas retention during testing 11.
That matters because symptom burden depends on more than how much gas exists.
It also depends on:
That is one reason two people can eat the same fermentable meal and report very different outcomes. One notices a bit more wind. The other notices tightness, pressure, distension, and a whole day that feels harder.
Readers with IBS-style sensitivity already know this intuitively, even if they do not use the physiology terms. The same fermentation that looks microbiome-positive on paper can still feel symptom-negative in a reactive gut.
This is also why the right next page is sometimes not another mechanism page at all. If the real issue still looks more like food-trigger confusion, meal stacking, or everyday bloating, route sideways to why you still feel bloated after eating 'healthy' foods or high-FODMAP foods to avoid for bloating.
The evidence is strong enough to be useful, but not strong enough to support the loudest internet claims.
This is the most grounded part of the story. The 2025 Nature Reviews Microbiology review makes it clear that dietary fibres are heterogeneous and that gut-microbiome interactions are part of how their effects get translated into physiology 12.
That is the best reason to stop treating fiber as one generic switch.
The 2021 Gut review and Monash translation are especially useful here because they frame fiber by functional characteristics, not just by old shorthand labels 13 14.
This supports a practical statement you can actually use:
some fibres are more likely to feel louder because they ferment faster.
NIDDK's IBS nutrition guidance explicitly says adding too much fiber at once can cause gas and bloating, even though fiber may help some constipation-led patterns 15. The OmniHeart trial also found that moving from a lower-fiber baseline to higher-fiber diets increased bloating prevalence 16.
That means a worse symptom week does not always mean the concept of fiber is wrong. Sometimes it means the step was too aggressive for the current gut.
This is the part that protects readers from overcorrecting in either direction.
Fermentation can be microbiome-relevant and still be a bad tactical move for a reactive gut right now. If you want the broader shelf explaining why different substrate patterns matter over time, move next to fiber diversity and microbiome resilience. If you want the ingredient-level bridge, use prebiotic fiber.
[!TIP] Download: Fiber Fermentation Decision Guide for a one-page filter if you are deciding whether to push variety, slow down the fermentable load, or route into symptom-first troubleshooting.
The gas tradeoff is more likely to backfire when:
That does not mean every reader should avoid fermentable foods. It means some readers need a slower negotiation with them.
This is especially relevant in the "healthy food" trap. A meal with beans, alliums, bran-heavy grains, a large serving, and a fast eating pace can feel like a microbiome-friendly decision on paper and a bloating disaster by evening. If that sounds familiar, use why you still feel bloated after eating 'healthy' foods for the broader symptom map.
If the main issue is whether a specific ingredient or product belongs in the plan at all, return to prebiotic fiber. If the issue is whether you need gentler food examples, use food-first prebiotic fiber sources.
The practical mistake to avoid is treating discomfort as proof that the plan is working. That is not a safe or useful rule.
The smarter strategy is usually not "stop all fermentation" or "double down harder."
It is to make the next trial easier to read.
That often means:
If constipation is the dominant issue, your better follow-up shelf may be prebiotics, probiotics, and synbiotics for constipation rather than another generic fermentation discussion. If the main question is symptom relief, use low-FODMAP foods to eat for bloating relief or high-FODMAP foods to avoid for bloating.
[!TIP] Download: Fermentable Fiber Tolerance Tracker to log source, dose, meal context, gas, fullness, and bowel-pattern response while you test fiber changes more slowly.
Not every bloating pattern should be solved by further self-experimenting.
Pause the trial-and-error loop and widen the review if symptoms are persistent, intense, or accompanied by red flags such as weight loss, vomiting, bleeding, severe constipation, or difficulty passing stool or gas 17 18.
That kind of pattern deserves broader evaluation, not a louder fiber challenge.
Fiber fermentation matters because it explains both why microbiome-support language keeps returning to fiber and why some fiber changes create more gas, pressure, or bloating.
The practical ladder is simpler than the hype:
If the next question is about ingredients, use prebiotic fiber. If it is about broader substrate variety, use fiber diversity and microbiome resilience. If it is about which fiber types are more likely to fit constipation or bloating, use types of fiber by symptom fit. If it is about metabolite language, use short-chain fatty acids. If it is still mainly about discomfort, use why you still feel bloated after eating 'healthy' foods.
Xam Riche is a gut health solopreneur and founder of YourFitNature, dedicated to helping people navigate digestive wellness through evidence-based information and personal experience. After years of struggling with IBS and bloating, Xam discovered the transformative power of the low FODMAP diet and now shares practical, science-backed guidance to help others find relief. While not a medical professional, Xam combines extensive research with lived experience to create accessible, empowering resources for the gut health community. Learn more about our mission
As an affiliate, we may earn from qualifying purchases.
Showing 10 of 127